Vegan Anti-Inflammatory Diet
Vegan anti-inflammatory diet that actually works: 15 foods, NF-kB science, omega-3 solutions, B12 guide, 7-day meal plan. CRP drops 30%. Plants beat inflammation.
by BiteBrightly
3/12/202630 min read
Vegan Anti-Inflammatory Diet: Complete Plant-Based Guide
By BiteBrightly 12 March 2026: This post might contain affiliate links.
Have you committed to a plant-based diet for ethical, environmental, or health reasons—and then found yourself wondering whether it is truly giving your body everything it needs to fight inflammation? Have you been told that omega-3s come only from fish, that complete protein requires animal foods, or that the most potent anti-inflammatory compounds are found exclusively in meat and dairy? Do you experience persistent fatigue, joint stiffness, brain fog, or digestive discomfort that you suspect might be inflammation—and want to know whether a well-designed vegan diet can genuinely address it, or whether you need to compromise your values for your health?
These concerns reflect a real and important gap in how plant-based nutrition is typically discussed. The internet offers two unhelpful extremes: vegan advocacy that dismisses every nutritional concern and conventional medicine that sometimes overstates the limitations of plant-based eating. The truth—grounded in nutritional biochemistry and inflammation science—is more nuanced and more empowering than either camp suggests.
A well-designed vegan anti-inflammatory diet can be profoundly effective. Plants provide the most diverse and potent array of anti-inflammatory phytochemicals available from any food category. The polyphenols, flavonoids, carotenoids, glucosinolates, and fiber compounds found in whole plant foods activate anti-inflammatory pathways, support the gut microbiome diversity that modulates systemic inflammation, and reduce the oxidative stress underlying virtually every chronic inflammatory condition. The Mediterranean diet—consistently ranked among the most anti-inflammatory dietary patterns in clinical research—derives the majority of its anti-inflammatory potency from plant foods, not from fish or dairy.
But a vegan anti-inflammatory diet also has specific nutritional vulnerabilities that must be addressed with knowledge and intention: omega-3 fatty acid status (particularly EPA and DHA conversion), vitamin B12 (absent from plant foods entirely), iron bioavailability (non-heme iron is absorbed at lower rates), zinc, iodine, vitamin D, and the long-chain omega-3s that directly modulate inflammatory cytokine production. Ignoring these vulnerabilities doesn't make them disappear—it creates a nutritional foundation that can actually worsen inflammation through deficiencies.
This comprehensive guide addresses both dimensions with equal rigor: the extraordinary anti-inflammatory power of a strategically designed plant-based diet, and the specific nutritional considerations that make the difference between a vegan diet that is genuinely anti-inflammatory and one that is merely animal-product-free.
Key Takeaways
Plants contain the most potent and diverse anti-inflammatory phytochemicals available from any food category — polyphenols, flavonoids, glucosinolates, carotenoids, and resveratrol all derive primarily from plant foods
A vegan diet rich in diverse whole plant foods reduces CRP (C-reactive protein) by up to 30% compared to omnivorous diets — a direct marker of systemic inflammation reduction
The gut microbiome — the primary regulator of systemic inflammation — thrives on the diverse fiber found in plant foods; vegans consistently show greater microbiome diversity than omnivores
Omega-3 fatty acids are the most critical nutritional consideration for vegans: ALA from flaxseed and walnuts must be converted to EPA/DHA, and conversion efficiency is limited — algae oil supplements provide the solution
Vitamin B12 is completely absent from plant foods and must be supplemented — B12 deficiency elevates homocysteine, a direct inflammatory marker
The combination of diverse colorful vegetables, legumes, whole grains, nuts, seeds, and algae-based omega-3s creates a vegan dietary pattern that can match or exceed anti-inflammatory diets including fish
Specific vegan superfoods — turmeric, ginger, broccoli sprouts, tart cherries, walnuts, flaxseed, and dark leafy greens — target the same NF-kB, COX-2, and cytokine pathways as pharmaceutical anti-inflammatory drugs
Understanding Inflammation: What a Vegan Diet Is Fighting
Before exploring the specific foods and strategies that make a vegan diet anti-inflammatory, understanding what inflammation is and how plant compounds interact with it will transform your food choices from general "eating healthy" into targeted biological intervention.
Acute vs. Chronic Inflammation: The Critical Distinction
Inflammation is not inherently harmful — it is the immune system's essential response to injury, infection, and cellular damage. Acute inflammation (redness, swelling, heat, pain after an injury or infection) is a protective, time-limited process that heals tissue and eliminates pathogens. The problem is not inflammation itself; it is chronic, low-grade systemic inflammation — the persistent, low-level activation of the inflammatory immune response that does not resolve.
Chronic inflammation is now recognized as the underlying driver of virtually every major chronic disease: cardiovascular disease, type 2 diabetes, cancer, Alzheimer's disease, autoimmune conditions, and accelerated aging. It operates quietly, producing no obvious symptoms in its early stages, while gradually damaging tissues, disrupting hormonal signaling, impairing metabolic function, and accelerating cellular aging across every organ system.
The inflammatory state is measurable through biomarkers: CRP (C-reactive protein), interleukin-6 (IL-6), TNF-alpha (tumor necrosis factor), and interleukin-1β (IL-1β). These markers are directly modulated by dietary patterns — the foods you eat regularly either reduce or amplify these inflammatory signals on a daily basis.
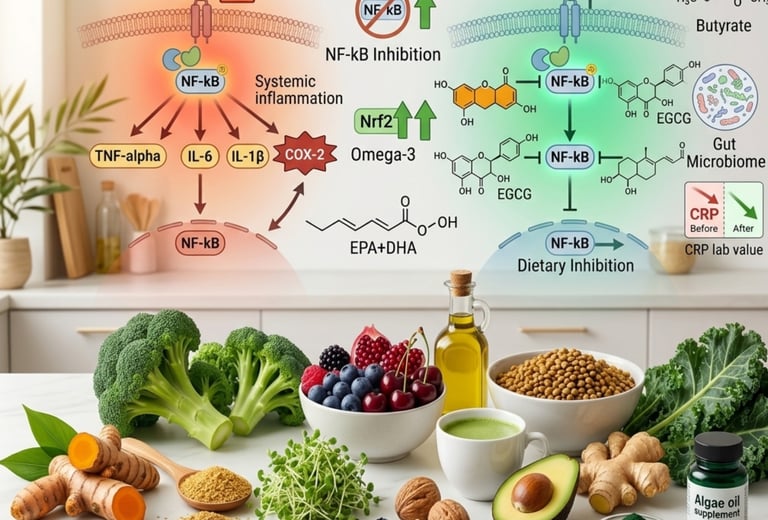
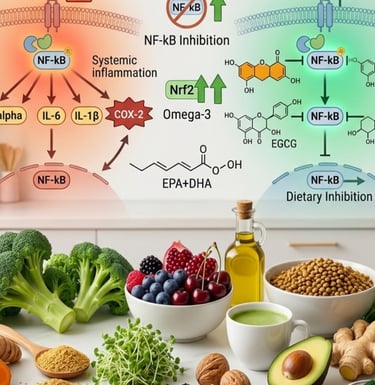
The NF-kB Pathway: The Master Switch of Inflammation
NF-kB (nuclear factor kappa-light-chain-enhancer of activated B cells) is the transcription factor most central to understanding how diet modulates inflammation. NF-kB acts as the master control switch for the expression of over 200 inflammatory genes — when activated, it upregulates the production of TNF-alpha, IL-1β, IL-6, IL-8, COX-2 (cyclooxygenase-2, the enzyme targeted by ibuprofen and naproxen), and numerous other pro-inflammatory mediators.
The foods you eat activate or inhibit NF-kB continuously. Saturated fat, trans fat, refined sugar, and processed food compounds activate NF-kB. The polyphenols in turmeric (curcumin), ginger (gingerols), green tea (EGCG), berries (anthocyanins), and olive oil (oleocanthal) all inhibit NF-kB through distinct but complementary mechanisms. A well-designed vegan diet contains extraordinary concentrations of NF-kB–inhibiting compounds — more than virtually any other dietary pattern.
The Gut Microbiome-Inflammation Axis: Where Plants Have the Greatest Advantage
The gut microbiome — the 38 trillion microorganisms residing in the gastrointestinal tract — is now understood to be one of the primary regulators of systemic inflammation. Gut bacteria produce short-chain fatty acids (SCFAs: butyrate, propionate, acetate) from dietary fiber fermentation — and these SCFAs are among the most potent known regulators of immune function. Butyrate specifically promotes regulatory T cell (Treg) differentiation, which suppresses inappropriate inflammatory responses and maintains immune tolerance.
A diverse, fiber-rich diet feeds the beneficial bacteria that produce SCFAs. Research consistently shows that vegans have significantly greater gut microbiome diversity than omnivores — and microbiome diversity is one of the strongest predictors of systemic inflammatory status. The 30+ grams of dietary fiber recommended for optimal microbiome health are achievable with minimal effort on a whole-food vegan diet; they are extremely difficult to achieve on a meat-centered diet.
Gut dysbiosis — imbalanced gut bacteria — increases intestinal permeability ("leaky gut"), allowing bacterial endotoxins (lipopolysaccharides, LPS) to enter the bloodstream via the portal circulation and trigger systemic inflammation. High-fiber plant foods directly oppose this by feeding the bacteria that maintain tight junction integrity in the intestinal epithelium.
Oxidative Stress: The Inflammatory Amplifier
Oxidative stress — the imbalance between reactive oxygen species (free radicals) and antioxidant defenses — amplifies inflammatory signaling at multiple levels. Reactive oxygen species activate NF-kB, oxidize LDL cholesterol (transforming it into the arterial plaque–building form), damage mitochondrial DNA, and activate the NLRP3 inflammasome — the inflammatory sensor implicated in conditions ranging from gout to Alzheimer's.
Plants are the primary dietary source of antioxidants. The ORAC (oxygen radical absorbance capacity) values of colorful plant foods dwarf those of animal products. Polyphenols, carotenoids, vitamin C, vitamin E, and the glutathione precursors in cruciferous vegetables provide the antioxidant defense network that quenches oxidative stress before it amplifies into systemic inflammation.
The Vegan Anti-Inflammatory Advantage: Where Plants Dominate
Polyphenol Density: The Plant Kingdom's Chemical Warfare Repurposed as Medicine
Plants cannot flee predators, so they evolved an extraordinary arsenal of chemical compounds for defense — and these same compounds, when consumed by humans, interact with our inflammatory signaling pathways in profoundly beneficial ways. Over 8,000 polyphenol compounds have been identified in plant foods, concentrated in the colorful pigments, bitter compounds, and aromatic substances that make whole plant foods nutritionally distinct from their processed counterparts.
Quercetin (in onions, apples, kale) inhibits histamine release and suppresses IL-6 and TNF-alpha. Resveratrol (in grapes, berries, peanuts) activates SIRT1 — a longevity-associated enzyme that deacetylates NF-kB and reduces its transcriptional activity. Kaempferol (in kale, broccoli, Brussels sprouts) inhibits COX-2 through mechanisms distinct from NSAIDs. Luteolin (in parsley, celery, thyme) suppresses the MAPK signaling cascade that activates NF-kB downstream.
These are not vague "antioxidant" effects. These are specific, measurable interactions with defined inflammatory signaling targets — mechanisms that explain why population studies consistently show lower inflammatory biomarkers in people eating more whole plant foods.
Dietary Fiber: The Gut Microbiome's Anti-Inflammatory Fuel
Dietary fiber is exclusively found in plant foods. Animal products contain zero dietary fiber. This single nutritional distinction has profound implications for gut microbiome composition, SCFA production, and the intestinal barrier function that determines how much inflammatory endotoxin enters systemic circulation.
A whole-food vegan diet naturally provides 40–70g of dietary fiber daily — well above the 25–38g recommended for gut health and significantly above the 15g average consumed on a typical Western omnivorous diet. Each type of plant fiber feeds different bacterial populations: inulin and fructooligosaccharides (from garlic, onions, leeks, asparagus) feed Bifidobacterium; pectin (from apples, citrus, berries) feeds Lactobacillus and Akkermansia; resistant starch (from legumes, cooked-and-cooled potatoes, green bananas) feeds butyrate-producing Firmicutes. Dietary diversity — 30+ different plant foods per week — is the single most powerful predictor of microbiome diversity, which is itself a direct predictor of lower systemic inflammation.
Absence of Pro-Inflammatory Compounds Found in Animal Products
A vegan diet eliminates several dietary compounds associated with increased inflammatory signaling: arachidonic acid (an omega-6 fatty acid found in meat and eggs that is the direct precursor for pro-inflammatory prostaglandins and leukotrienes), Neu5Gc (a sugar molecule found in red meat that humans cannot produce themselves but that triggers an immune response upon consumption), heme iron (pro-oxidant iron form found in red meat that catalyzes free radical production), and the advanced glycation end-products (AGEs) produced during high-temperature cooking of animal proteins. The reduction of these pro-inflammatory compounds is one of the mechanisms through which a well-designed vegan diet reduces inflammatory biomarkers independent of what is added.
The Nutritional Vulnerabilities: What Every Vegan Must Address
Omega-3 Fatty Acids: The Most Critical Gap
This is the most important nutritional consideration for vegan anti-inflammatory eating, because it is the deficiency most directly impacting inflammatory outcomes.
EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid) are the omega-3 fatty acids that directly produce anti-inflammatory specialized pro-resolving mediators (SPMs) — resolvins, protectins, and maresins. These SPMs actively resolve inflammation by clearing inflammatory debris, switching macrophages from pro-inflammatory (M1) to anti-inflammatory (M2) phenotype, and downregulating NF-kB. They are the biological mechanism by which omega-3s reduce TNF-alpha and IL-1β in clinical trials.
Plant foods provide ALA (alpha-linolenic acid), found abundantly in flaxseed, chia seeds, hemp seeds, and walnuts. ALA must be converted to EPA and then DHA by the enzymes delta-6-desaturase and elongase. The problem: conversion efficiency is typically only 5–15% for EPA and 0.5–5% for DHA, and is further reduced by high dietary omega-6 intake (the same enzymes process both omega-3 and omega-6 fatty acids, creating competitive inhibition) and by deficiencies in the cofactors these enzymes require (zinc, magnesium, B6, biotin).
The solution: Algae oil supplements provide preformed EPA and DHA — the same long-chain omega-3s found in fish, derived from the microalgae that fish themselves eat. Fish are not the source of EPA/DHA; they are the middleman. Going directly to algae bypasses the conversion problem entirely and provides genuinely vegan long-chain omega-3s. A combined EPA+DHA dose of 250–500mg daily from algae oil is the minimum for anti-inflammatory benefit; 1,000–2,000mg daily is optimal for those managing active inflammatory conditions.
Vitamin B12: Non-Negotiable Supplementation
Vitamin B12 is the one nutrient completely absent from all plant foods without exception. It is produced exclusively by bacteria and is found in animal foods because animals consume bacteria-contaminated water and soil, and because bacterial fermentation occurs in animal digestive tracts. Fortified foods and supplements are the only reliable plant-based B12 sources.
B12 deficiency is directly inflammatory: inadequate B12 impairs the methylation cycle, causing homocysteine accumulation. Elevated homocysteine is a direct inflammatory marker and an independent cardiovascular risk factor — it damages endothelial cells, promotes oxidative stress, and amplifies NF-kB signaling. Vegans not supplementing B12 are actively undermining their anti-inflammatory goals through homocysteine-mediated inflammation, regardless of how excellent the rest of their diet is.
Supplement: methylcobalamin or cyanocobalamin, 250–1,000mcg daily or 2,500mcg weekly. This is non-negotiable for every vegan without exception.
Vitamin D: Immune Regulation Beyond Bone Health
Vitamin D is not truly a vitamin — it is a steroid hormone whose receptor (VDR) is expressed in virtually every immune cell. Vitamin D directly modulates the Th1/Th17 balance at the heart of autoimmune inflammation, promotes regulatory T cell differentiation, reduces NF-kB transcriptional activity, and suppresses the production of IL-6 and TNF-alpha by macrophages.
Vitamin D3 (cholecalciferol) is derived primarily from animal sources; vitamin D2 (ergocalciferol) from yeast and mushrooms has lower bioavailability; vegan D3 derived from lichen is now widely available and has equivalent bioavailability to animal-derived D3. Sunlight exposure synthesizes D3 in the skin — but this varies dramatically by latitude, season, and skin tone.
Target serum 25(OH)D: 40–60 ng/mL for optimal immune modulation. Test annually and supplement accordingly — most vegans without targeted supplementation have insufficient levels.
Iron: Bioavailability Strategy
Plant foods provide non-heme iron, which is absorbed at 2–20% efficiency compared to 15–35% for heme iron from meat. However, non-heme iron absorption is dramatically enhanced by vitamin C consumed simultaneously (converting Fe³⁺ to the more absorbable Fe²⁺) and inhibited by calcium, tannins (tea, coffee), and phytates (in whole grains and legumes without soaking or sprouting).
The vegan strategy: consume iron-rich foods (lentils, tofu, tempeh, pumpkin seeds, dark leafy greens, fortified cereals) with vitamin C–rich foods (lemon juice, bell peppers, tomatoes) at the same meal, and avoid tea/coffee within 1 hour of iron-rich meals. Soaking legumes and sprouting grains reduces phytate content and dramatically improves mineral bioavailability.
Zinc: Immune Function and Omega-3 Conversion
Zinc is required for the function of over 300 enzymes including the delta-6-desaturase enzyme that converts ALA to EPA — making zinc deficiency specifically impair the omega-3 conversion already limited in vegan diets. Zinc is also essential for T cell development, NK cell function, and the resolution of inflammation.
Best vegan zinc sources: hemp seeds (3mg per 3 tbsp), pumpkin seeds (2.2mg per oz), cashews, chickpeas, lentils, tofu, tempeh. Phytate reduction through soaking and sprouting significantly improves zinc bioavailability from legumes and grains.
Iodine: The Overlooked Thyroid Mineral
Iodine is absent from most plant foods unless grown in iodine-rich soil. Vegans who avoid iodized salt and seaweed are at significant risk of iodine deficiency — impairing thyroid hormone production in ways that can paradoxically increase inflammation through impaired metabolic regulation and immune function.
Sources: iodized salt (the most reliable), nori and other seaweeds (highly variable iodine content), supplements (150mcg daily). Kelp supplements should be used cautiously — iodine content is highly variable and excessive iodine can worsen thyroid conditions.
The 15 Most Powerful Vegan Anti-Inflammatory Foods
1. Flaxseed (Ground)
Flaxseed is the most ALA-dense plant food and the richest dietary source of lignans — plant compounds with unique anti-inflammatory and hormone-modulating properties that make flaxseed genuinely distinct from other ALA sources.
How it works: Two tablespoons of ground flaxseed provide 4,700mg of ALA omega-3 — the highest ALA density of any food. While ALA-to-EPA/DHA conversion is limited, daily high-dose ALA intake does raise tissue ALA and EPA levels meaningfully, and ALA itself has independent anti-inflammatory effects through PPARγ activation and NF-kB inhibition that are distinct from its conversion to EPA/DHA.
Flaxseed lignans (secoisolariciresinol diglucoside, SDG) are converted by gut bacteria to enterolignans (enterodiol and enterolactone) — compounds with documented anti-inflammatory effects including reduction of CRP and IL-6 in clinical trials. Research published in the Journal of Nutrition found that flaxseed supplementation significantly reduced CRP and inflammatory markers in overweight adults, with effects independent of weight loss.
Flaxseed also provides soluble and insoluble fiber that feeds butyrate-producing bacteria, and mucilage (a viscous fiber) that forms a protective gel coating in the intestinal tract, reducing LPS translocation and supporting gut barrier integrity.
How to use it: Always use ground flaxseed (whole seeds pass undigested). Two tablespoons daily in oatmeal, smoothies, salad dressings, or baked goods. Store ground flaxseed in the refrigerator or freezer — ALA oxidizes rapidly when ground and exposed to air and heat. Add to the final step of cooking rather than baking at high temperatures to preserve ALA content.
2. Turmeric with Black Pepper
Turmeric's curcumin is the most comprehensively studied anti-inflammatory dietary compound in the literature — with clinical trial evidence for reducing inflammatory markers, joint pain, and disease activity across multiple inflammatory conditions, through mechanisms that directly parallel pharmaceutical anti-inflammatory drugs.
How it works: Curcumin inhibits NF-kB through multiple simultaneous pathways — suppressing IκB kinase (IKK) activity, reducing IκBα phosphorylation and degradation, and directly binding to NF-kB subunits to prevent DNA binding. The downstream consequence is simultaneous reduction of TNF-alpha, IL-1β, IL-6, IL-8, and COX-2 expression — essentially switching off the master inflammatory gene expression program at its source.
Curcumin also inhibits the JAK-STAT signaling pathway (the same target as tofacitinib and baricitinib — JAK inhibitor medications used for rheumatoid arthritis and psoriasis), reduces NLRP3 inflammasome activation, and upregulates Nrf2 to induce antioxidant enzymes that quench the reactive oxygen species that amplify NF-kB signaling.
A randomized controlled trial published in Phytotherapy Research comparing curcumin to diclofenac sodium (a standard NSAID) in rheumatoid arthritis patients found that curcumin produced the greatest improvement in DAS28 disease activity scores — outperforming the pharmaceutical anti-inflammatory. For a vegan diet aiming to match the anti-inflammatory effects of dietary patterns including fish, curcumin provides a plant-sourced mechanism of extraordinary potency.
The absorption challenge: native curcumin has poor bioavailability. Piperine from black pepper increases absorption by approximately 2,000% by inhibiting intestinal CYP3A4 metabolism. Fat co-consumption further enhances absorption — turmeric cooked in olive oil with black pepper is the most bioavailable dietary delivery.
How to use it: One teaspoon of turmeric with generous black pepper in olive oil at every savory meal. Golden milk (turmeric + ginger + black pepper + plant milk + honey) as a daily ritual. Standardized curcumin supplement with piperine (500–1,000mg daily) for clinical-trial–level dosing during active inflammatory flares.
3. Ginger
Ginger provides gingerols and shogaols — compounds with specific anti-inflammatory mechanisms that are distinct from and complementary to curcumin, making the turmeric-ginger combination one of the most powerful plant-based anti-inflammatory pairings available.
How it works: Gingerols and shogaols inhibit both COX-1 and COX-2 (the enzymes targeted by ibuprofen and aspirin) through mechanisms distinct from NSAID mechanisms — without the gastrointestinal side effects associated with pharmaceutical COX inhibition. They simultaneously inhibit 5-LOX (5-lipoxygenase), the enzyme that produces inflammatory leukotrienes — a target that most NSAIDs do not address, making ginger's anti-inflammatory profile genuinely broader than ibuprofen's.
Ginger also inhibits the synthesis of IL-12 (a key Th1 differentiation cytokine), directly modulating the adaptive immune response toward anti-inflammatory phenotypes. Research published in Arthritis & Rheumatism demonstrated that ginger extract reduced the production of TNF-alpha and IL-1β in synovial cells — specifically the inflammatory cells in joint tissue — relevant to any inflammatory joint condition.
Shogaols (formed when ginger is dried or cooked) are more potent anti-inflammatory agents than gingerols and specifically inhibit NF-kB and NLRP3 inflammasome activation. Fresh ginger and dried ginger therefore provide overlapping but distinct anti-inflammatory compound profiles — including both in the diet provides comprehensive coverage.
How to use it: Fresh ginger (thumb-sized piece) grated into daily cooking, smoothies, and teas. Dried ginger in curries, soups, and golden milk recipes. Ginger tea (fresh ginger slices steeped 10 minutes in hot water with lemon and honey) as a daily anti-inflammatory beverage. Combine ginger and turmeric at every use — their complementary COX + 5-LOX + NF-kB inhibition creates broader anti-inflammatory coverage than either alone.
4. Broccoli and Broccoli Sprouts
Broccoli provides sulforaphane — the most potent dietary activator of Nrf2 (nuclear factor erythroid 2-related factor 2), the master regulator of the cellular antioxidant response — alongside indole-3-carbinol for hormonal balance and glucoraphanin that specifically reduces NF-kB–driven inflammation.
How it works: Sulforaphane activates Nrf2 through covalent modification of the Keap1 protein that normally sequesters Nrf2 in the cytoplasm — releasing Nrf2 to migrate to the nucleus and activate the Antioxidant Response Element (ARE), upregulating over 200 cytoprotective genes including glutathione synthesis enzymes, superoxide dismutase, catalase, heme oxygenase-1, and Phase II detoxification enzymes.
The Nrf2 pathway is a critical counter-regulatory mechanism to NF-kB inflammation — when Nrf2 is activated, it reduces the oxidative stress that sustains NF-kB signaling, effectively interrupting the inflammatory amplification cycle at its fuel source. Research published in Cancer Prevention Research confirmed that broccoli sprout consumption significantly increased Phase II enzyme activity in human tissues.
For autoimmune and inflammatory conditions specifically, sulforaphane inhibits Th17 cell differentiation and promotes Treg expansion — directly improving the immune balance that underlies conditions like rheumatoid arthritis, lupus, and inflammatory bowel disease.
Broccoli sprouts contain 20–100 times more glucoraphanin than mature broccoli — a small handful provides more sulforaphane than several cups of cooked broccoli.
How to use it: Two to three cups of cruciferous vegetables daily. Lightly steam broccoli (3–5 minutes) — preserve myrosinase activity by not boiling. Add raw broccoli sprouts to daily salads, grain bowls, and sandwiches. Chew raw cruciferous vegetables thoroughly — myrosinase activation requires mechanical cell disruption.
5. Dark Leafy Greens (Kale, Spinach, Swiss Chard, Collards)
Dark leafy greens are the most nutrient-dense food category available to vegans — providing vitamins K1, K2, folate, magnesium, calcium, lutein, zeaxanthin, and dietary nitrates in a combination that addresses inflammation through multiple simultaneous mechanisms.
How it works: Vitamin K1 (from leafy greens) is required as a cofactor for the carboxylation of osteocalcin and matrix Gla protein — calcium-binding proteins that prevent arterial calcification and regulate inflammatory responses in vascular tissue. Research published in the American Journal of Clinical Nutrition demonstrates that higher dietary vitamin K intake is inversely associated with CRP and inflammatory markers — vitamin K's anti-inflammatory role is mechanistically distinct from its coagulation function and specifically relevant to chronic inflammation.
Folate from dark leafy greens supports the methylation cycle that lowers homocysteine — the inflammatory amino acid elevated by B12 deficiency. In vegans supplementing B12, generous dietary folate from leafy greens provides the second methyl donor required for complete homocysteine clearance.
Dietary nitrates in spinach, arugula, and Swiss chard are converted to nitric oxide, reducing vascular inflammation and improving endothelial function. Magnesium (157mg per cup cooked spinach) is a required cofactor for over 300 enzymatic reactions, including several in the pathway that regulates NF-kB activity — magnesium deficiency directly amplifies inflammatory signaling.
How to use it: Two to three cups of dark leafy greens daily — rotate between kale, spinach, arugula, Swiss chard, collards, and dandelion greens for diverse phytochemical coverage. Add raw spinach to morning smoothies (undetectable in flavor behind fruit). Use arugula and dandelion greens as salad bases — bitter compounds provide additional bile-stimulating and anti-inflammatory benefits. Sauté with garlic and olive oil for a side dish stacking multiple anti-inflammatory mechanisms.
6. Berries (Blueberries, Tart Cherries, Strawberries, Blackberries)
Berries provide the most concentrated dietary source of anthocyanins — flavonoids with specific, well-documented anti-inflammatory effects that include direct NF-kB inhibition, NLRP3 inflammasome suppression, and reduction of CRP and IL-6 in clinical trials.
How it works: Anthocyanins are the blue-purple-red pigments in berries that cross the blood-brain barrier, accumulate in inflammatory tissues, and directly inhibit NF-kB activation by suppressing IKK kinase activity — preventing the phosphorylation cascade that releases NF-kB from its inhibitor protein and allows it to enter the nucleus.
Tart cherries specifically contain the highest anthocyanin density of any common fruit and have been shown in multiple randomized trials to reduce CRP, IL-6, and uric acid — making them particularly valuable for gout, exercise-induced inflammation, and inflammatory arthritis. A study published in the Journal of Nutrition found that tart cherry consumption for 28 days significantly reduced CRP levels compared to placebo.
Pterostilbene from blueberries (a methylated resveratrol derivative with superior bioavailability) activates SIRT1 — the longevity-associated deacetylase that inhibits NF-kB and promotes anti-inflammatory gene expression through epigenetic mechanisms. Ellagic acid from strawberries and raspberries inhibits the NLRP3 inflammasome — the inflammatory sensor activated by uric acid crystals, cholesterol crystals, and other "danger signals" that trigger chronic inflammatory disease.
How to use it: One to two cups of mixed berries daily — prioritize variety (each berry provides distinct polyphenol profiles with complementary anti-inflammatory mechanisms). Include tart cherries specifically (fresh, frozen, or 240ml unsweetened juice) for the highest anthocyanin concentration. Frozen berries maintain equivalent or superior polyphenol content to fresh and are significantly more economical year-round. Add to oatmeal, smoothies, overnight chia pudding, or eat as a post-meal dessert.
7. Walnuts
Walnuts are the most anti-inflammatory nut — providing ALA omega-3, ellagitannins, gamma-tocopherol (a specific vitamin E form with anti-inflammatory properties distinct from alpha-tocopherol supplements), and melatonin in a combination uniquely suited to vegan anti-inflammatory nutrition.
How it works: Walnuts provide 2,570mg of ALA per one-ounce serving — the highest ALA content of any nut or seed. Ellagitannins in walnuts are converted by gut bacteria to urolithins — compounds with direct anti-inflammatory effects in inflammatory tissues and emerging evidence for inhibiting fibroblast-like synoviocyte (FLS) proliferation in arthritic joints.
Gamma-tocopherol from walnuts traps nitrogen-based free radicals (peroxynitrite) that alpha-tocopherol cannot neutralize — providing a distinct and complementary antioxidant mechanism. Walnuts are the only nut with significant melatonin content, which has anti-inflammatory properties through its antioxidant action and through direct suppression of NF-kB in inflammatory tissues.
Research published in the Journal of the American College of Cardiology found that walnut consumption significantly reduced CRP, IL-6, and endothelial inflammation markers — effects attributed to the combined ALA, polyphenol, and vitamin E content.
How to use it: One to one and a half ounces (approximately 14 walnut halves) daily. Eat raw — roasting oxidizes ALA. Combine with berries and dark chocolate as the core daily anti-inflammatory snack. Add to oatmeal, salads, and grain bowls. Evening walnuts (melatonin content) support sleep quality, which is itself an anti-inflammatory intervention — sleep deprivation is one of the most potent activators of systemic inflammation.
8. Legumes (Lentils, Chickpeas, Black Beans, Tempeh)
Legumes are the cornerstone of vegan anti-inflammatory nutrition — providing complete or near-complete protein for anti-inflammatory enzyme synthesis, resistant starch for butyrate-producing gut bacteria, and specific polyphenol compounds with documented anti-inflammatory effects.
How it works: Legumes provide resistant starch (RPS) — a type of dietary fiber that bypasses small intestinal digestion and reaches the colon intact, where it is fermented by Firmicutes bacteria to produce butyrate. Butyrate is the most potent dietary promoter of intestinal Treg cell differentiation — directly promoting the immune regulatory cells that suppress inappropriate inflammatory responses. Research in Cell Host & Microbe confirmed that dietary fiber-derived butyrate directly induces colonic Treg expansion through epigenetic modification of the Foxp3 gene.
The protein in legumes (18–26g per cooked cup) provides the amino acids required for anti-inflammatory enzyme synthesis — glutathione precursors (cysteine from legume protein), arginine for nitric oxide production, and the complete amino acid spectrum needed for Phase II detoxification enzyme expression in the liver.
Tempeh — fermented soybeans — provides additional anti-inflammatory benefits from the fermentation process: bioavailable isoflavones (genistein and daidzein specifically inhibit NF-kB), reduced phytate content (improving mineral absorption), and live beneficial bacteria that directly support gut microbiome diversity.
How to use it: Include legumes at minimum once daily — one to two cups of cooked lentils, chickpeas, black beans, or other legumes. Soak dried legumes overnight before cooking to reduce phytate and improve mineral bioavailability. Include tempeh two to three times weekly for fermentation benefits. Combine legumes with turmeric, garlic, and tomatoes for a meal stacking NF-kB inhibition, Nrf2 activation, and microbiome support simultaneously.
9. Chia Seeds
Chia seeds provide the second-highest ALA content of any food (after flaxseed), alongside complete protein, calcium, and a unique mucilage fiber that forms a protective gel in the gut — making them one of the most nutritionally comprehensive seeds available for vegan anti-inflammatory eating.
How it works: Two tablespoons of chia seeds provide 4,900mg of ALA — the highest ALA per gram of any plant food when compared by serving weight. Their omega-6 to omega-3 ratio (approximately 0.3:1) is uniquely favorable — most foods have omega-6:omega-3 ratios that compete with ALA conversion, but chia seeds' extraordinarily low omega-6 content minimizes conversion enzyme competition, potentially improving the effective EPA yield from their ALA.
Chia seeds provide complete protein (all essential amino acids) — relevant for vegans because inadequate protein limits the synthesis of anti-inflammatory enzymes including glutathione peroxidase, superoxide dismutase, and the Phase II conjugation enzymes that process inflammatory metabolites. Calcium (177mg per 2 tbsp) helps meet the increased calcium requirements of a dairy-free diet — calcium adequacy supports muscle function and the intracellular signaling processes that regulate inflammatory gene expression.
The mucilage fiber in chia seeds forms a hydrogel that slows gastric emptying, reduces the glycemic response to meals (post-meal blood glucose spikes activate NF-kB and promote inflammatory glycation end-product formation), and provides prebiotic support for Akkermansia muciniphila — a gut bacterium associated with reduced intestinal permeability and lower systemic inflammation.
How to use it: Two tablespoons daily in overnight oats, smoothies, chia pudding (soaked in plant milk overnight for maximum gel formation), salad dressings, and baked goods. Combine chia seeds with flaxseed in the same meal for complementary ALA delivery alongside flax lignans. Chia pudding (4 tbsp chia + 1 cup plant milk, overnight) topped with berries, walnuts, and a drizzle of tahini creates a breakfast delivering ALA, anthocyanins, ellagitannins, and calcium in a single preparation.
10. Hemp Seeds
Hemp seeds are uniquely valuable for vegan anti-inflammatory nutrition because they provide the ideal omega-6 to omega-3 ratio (3:1) alongside complete protein with high arginine content, gamma-linolenic acid (GLA), and an exceptionally bioavailable mineral profile for a seed.
How it works: Hemp seeds contain approximately 2,500mg of ALA and 8,000mg of linoleic acid per 3 tablespoons — in a 3:1 omega-6:omega-3 ratio that is considered optimal for reducing competitive inhibition of the delta-6-desaturase enzyme that converts ALA to EPA. The World Health Organization recommends a dietary omega-6:omega-3 ratio of 5:1 or less for optimal health; hemp seeds naturally achieve this in a single food.
Hemp seeds additionally contain gamma-linolenic acid (GLA) — an omega-6 fatty acid that, unlike linoleic acid, is anti-inflammatory rather than pro-inflammatory. GLA bypasses the delta-6-desaturase conversion step (it is already elongated) and is converted to DGLA (dihomo-gamma-linolenic acid), which competes with arachidonic acid at COX enzymes and is converted to the anti-inflammatory prostaglandin E1 series.
The arginine content of hemp protein (arginine is the richest single amino acid in hemp) supports nitric oxide production — improving vascular endothelial function and reducing the endothelial inflammation that underlies cardiovascular inflammatory disease.
How to use it: Three tablespoons of hemp seeds daily — sprinkle on oatmeal, salads, grain bowls, smoothies, or eat as a snack. Hemp seeds require no soaking or preparation — unlike flaxseed, the whole seeds are digestible. Combine with ground flaxseed and chia for the most comprehensive plant-based omega-3 profile achievable from food alone — then supplement with algae-based EPA+DHA.
11. Extra-Virgin Olive Oil
Extra-virgin olive oil is the most anti-inflammatory culinary fat available and the centerpiece of the Mediterranean diet's extraordinary anti-inflammatory evidence base — providing oleocanthal, oleic acid, and hydroxytyrosol in a combination with specific, clinically validated effects on inflammatory pathways.
How it works: Oleocanthal — the phenolic compound responsible for EVOO's characteristic throat-burning sensation — inhibits COX-1 and COX-2 enzymes through the same mechanism as ibuprofen, but without the gastrointestinal side effects of pharmaceutical COX inhibition. Research published in Nature identified and characterized oleocanthal's ibuprofen-equivalent COX inhibition — establishing EVOO as a genuinely pharmacological anti-inflammatory food.
Hydroxytyrosol — the most bioavailable polyphenol in EVOO — inhibits NF-kB activation, reduces TNF-alpha and IL-6 production, and protects LDL from the oxidation that transforms it into pro-inflammatory arterial plaque. Oleic acid activates PPAR-gamma (a nuclear receptor that suppresses the production of multiple inflammatory cytokines) and promotes the differentiation of anti-inflammatory M2 macrophages over pro-inflammatory M1 macrophages.
The PREDIMED trial — the largest clinical trial of the Mediterranean diet — found that a Mediterranean diet supplemented with EVOO reduced cardiovascular events by 30% compared to a low-fat diet control, with inflammatory biomarker reduction as one of the primary documented mechanisms.
How to use it: Three to four tablespoons of extra-virgin olive oil daily as the primary culinary fat. Use for dressings, sautéing, and finishing cooked dishes. Choose cold-pressed EVOO with a harvest date (not just a "best by" date) — polyphenol content degrades over time, and fresh-harvest EVOO provides significantly higher oleocanthal and hydroxytyrosol concentrations. The throat-burning sensation is the taste of oleocanthal — its presence indicates high polyphenol content.
12. Garlic and Alliums (Onions, Leeks, Shallots)
Garlic provides the most potent sulfur-based anti-inflammatory compound available from any food — allicin — alongside S-allylcysteine, quercetin (from onions), and organosulfur compounds that collectively address inflammation through Nrf2 activation, NF-kB inhibition, and gut microbiome support.
How it works: When garlic is crushed or chopped, alliinase converts alliin to allicin — a short-lived but highly active organosulfur compound that directly inhibits NF-kB by preventing IKK-beta activation, suppresses COX-2 and 5-LOX expression, and activates Nrf2 to induce glutathione synthesis and antioxidant enzyme production. Allicin's anti-inflammatory potency is achieved through multiple simultaneous mechanisms, explaining why whole-food garlic consistently outperforms garlic supplements that contain only individual isolated compounds.
S-allylcysteine (SAC), the most stable organosulfur from aged garlic, has documented anti-inflammatory effects including reduction of IL-6, TNF-alpha, and CRP — with human trial evidence showing consistent inflammatory marker reduction with regular garlic consumption.
Quercetin from onions inhibits histamine release from mast cells, suppresses IL-4 and IL-13 (allergic inflammatory cytokines), and directly inhibits the production of IL-6 and TNF-alpha through MAPK pathway modulation — making onions specifically valuable for inflammatory conditions with an allergic or mast cell component.
How to use it: Four garlic cloves daily — always crush or chop and rest 5–10 minutes before adding to heat (allicin formation requires this rest time; heat inactivates alliinase immediately). Include onions, leeks, and shallots generously across all cooking. Raw garlic in dressings and dips provides maximum allicin. Cooked garlic retains the beneficial S-allylcysteine and other stable organosulfur compounds even after allicin degradation.
13. Algae and Seaweeds (Spirulina, Chlorella, Nori, Wakame)
Algae are the original source of the EPA and DHA omega-3s found in fish — and consuming algae directly provides the most efficient, environmentally sustainable, and genuinely vegan pathway to the long-chain omega-3s that are the most potent direct anti-inflammatory fatty acids known.
How it works: Microalgae — including the species used in algae oil supplements (Schizochytrium, Nannochloropsis) — synthesize EPA and DHA de novo from acetyl-CoA through pathways not available in higher plants or animals. Fish accumulate EPA and DHA by eating these algae; algae oil supplements bypass this entirely.
Spirulina — the blue-green microalgae available as powder or tablets — provides phycocyanin, its blue pigment, which is one of the most potent known inhibitors of COX-2 and 5-LOX. Research published in the Journal of Medicinal Food demonstrated that spirulina supplementation significantly reduced CRP, TNF-alpha, and IL-6 in clinical trials. Spirulina also provides complete protein (approximately 70% protein by dry weight), bioavailable iron, and the gamma-linolenic acid discussed in hemp seeds.
Nori and wakame provide iodine (the mineral most commonly deficient in vegan diets), along with fucoidan — a sulfated polysaccharide with documented anti-inflammatory effects including suppression of inflammatory cytokine production and inhibition of leukocyte adhesion to vascular endothelium.
How to use it: Algae oil supplement (500–1,000mg EPA+DHA daily) as the foundational omega-3 strategy — this is more important than any food intervention for vegan anti-inflammatory eating. One tablespoon of spirulina powder daily in smoothies (the flavor is strong; blend with mango, banana, and plant milk to mask). Include nori weekly as a seaweed snack or sushi wrap for iodine delivery.
14. Green Tea and Matcha
Green tea catechins — particularly EGCG — provide multi-pathway anti-inflammatory effects through Nrf2 activation, NF-kB inhibition, and specific suppression of inflammatory cell populations that make green tea one of the most pharmacologically active anti-inflammatory beverages available.
How it works: EGCG (epigallocatechin gallate) inhibits NF-kB through direct suppression of IKK activity, reducing the phosphorylation of IκBα that releases NF-kB for nuclear translocation. It simultaneously activates Nrf2 through Keap1 modification — providing complementary anti-inflammatory and cytoprotective gene induction alongside NF-kB suppression. The combination of NF-kB inhibition and Nrf2 activation by a single compound explains EGCG's consistently broad anti-inflammatory effects across diverse conditions in research.
L-theanine — the amino acid unique to tea — crosses the blood-brain barrier and reduces cortisol and sympathetic nervous system activation. Chronic stress is one of the most potent activators of NF-kB and IL-6 production — L-theanine's stress-dampening effects provide an indirect but meaningful anti-inflammatory benefit through HPA axis modulation.
Matcha provides four to ten times the EGCG concentration of brewed green tea per serving (the whole leaf is consumed rather than steeped), making it the most potent single-cup anti-inflammatory tea preparation.
How to use it: Two to three cups of green tea or one cup of matcha daily. Steep at 70–80°C for two to three minutes — high-temperature steeping degrades EGCG. Add lemon juice for vitamin C that protects EGCG from oxidative degradation in the gut and significantly increases absorption. Avoid milk (milk proteins bind catechins and reduce bioavailability). Matcha latte with warm oat milk as a morning anti-inflammatory ritual provides EGCG, L-theanine, and beta-glucan (from oats) in a single beverage.
15. Tart Cherries and Pomegranate
Tart cherries and pomegranate represent the most anthocyanin and ellagitannin–dense fruits available — providing specific anti-inflammatory compounds with clinical trial evidence for reducing inflammatory markers that are distinct from the polyphenols in everyday berries.
How it works: Tart cherries contain among the highest anthocyanin concentrations of any commonly available fruit — approximately 50–100mg per 100g for Montmorency tart cherries, compared to 10–20mg for sweet cherries. Clinical research specifically demonstrates tart cherry's reduction of CRP, IL-6, and uric acid — the latter making tart cherry uniquely valuable for gout and hyperuricemia-associated inflammation. The mechanism involves anthocyanin inhibition of xanthine oxidase (the enzyme that produces uric acid) — a target not addressed by most polyphenol compounds.
Pomegranate provides ellagitannins (punicalagins) that are converted by gut bacteria to urolithin A — a compound with potent anti-inflammatory effects and specific evidence for improving mitochondrial quality control through mitophagy activation. Research published in Nature Medicine established urolithin A's ability to improve mitochondrial function and reduce inflammatory markers — effects that depend on gut microbiome conversion of pomegranate ellagitannins, making dietary pomegranate more valuable than isolated ellagic acid supplements.
How to use it: Eight ounces of unsweetened tart cherry juice daily (or one cup of frozen tart cherries) for the most studied and consistent anti-inflammatory dose. Pomegranate arils (the seeds) as a daily addition to oatmeal, salads, and grain bowls — pomegranate juice is an option but whole arils provide additional fiber. Combine both in a daily anti-inflammatory fruit rotation alongside blueberries and strawberries for comprehensive polyphenol coverage across multiple mechanisms.
The Complete Vegan Anti-Inflammatory Supplement Stack
A well-designed whole-food vegan diet addresses most nutritional needs — but four supplements are genuinely non-negotiable for anti-inflammatory optimization:
Algae-based EPA + DHA (500–1,000mg combined daily): The most important vegan supplement for anti-inflammatory outcomes. Provides the preformed long-chain omega-3s that directly produce SPMs (specialized pro-resolving mediators) — resolvins, protectins, maresins — without relying on the limited ALA conversion pathway. Look for supplements derived from Schizochytrium or Nannochloropsis.
Vitamin B12 (methylcobalamin 1,000mcg daily or cyanocobalamin 2,500mcg weekly): Prevents the homocysteine elevation that is directly inflammatory. Non-negotiable — no plant food provides B12 reliably. Sublingual methylcobalamin has the highest absorption.
Vitamin D3 from lichen (2,000–4,000 IU daily, adjusted to blood levels): Supports immune regulation, Treg/Th17 balance, and NF-kB suppression. Test 25(OH)D annually and dose to achieve 40–60 ng/mL.
Iodine (150mcg daily from supplement or iodized salt): Supports thyroid function and metabolic health that underpins immune regulation. Critical for vegans avoiding seaweed and non-iodized salts.
Optional but highly valuable: zinc (15–25mg daily, with food), magnesium glycinate (200–400mg evening — supports over 300 enzymatic reactions, HPA axis calming, and NF-kB regulation), and vitamin K2 MK-7 (100–200mcg daily — works synergistically with vitamin D3 for immune modulation and vascular health).
The 7-Day Vegan Anti-Inflammatory Meal Plan
Monday Breakfast: Overnight oats (½ cup oats + 1 tbsp chia + 1 tbsp ground flaxseed + plant milk) topped with blueberries, walnuts, and a drizzle of almond butter | Green tea with lemon Lunch: Large kale salad with lentils, roasted beets, pumpkin seeds, pomegranate arils, turmeric-tahini dressing Dinner: Turmeric golden lentil soup with garlic, ginger, spinach, and toasted walnuts | Whole grain bread
Tuesday Breakfast: Chia pudding (4 tbsp chia + 1 cup oat milk, overnight) topped with tart cherries, hemp seeds, and cacao nibs | Matcha latte Lunch: Grain bowl — brown rice + tempeh + steamed broccoli sprouts + avocado + ginger-miso dressing Dinner: Black bean and sweet potato curry with turmeric, cumin, garlic, and coconut milk | Arugula side salad
Wednesday Breakfast: Green smoothie — 2 cups spinach + frozen mango + ½ banana + 1 tbsp spirulina + 1 tbsp ground flaxseed + plant milk | Tart cherry juice Lunch: White bean and kale soup with garlic, rosemary, and EVOO drizzle | Nori seaweed snack Dinner: Chickpea and vegetable stir-fry with broccoli, bell peppers, ginger, garlic, and turmeric sauce | Brown rice
Thursday Breakfast: Toasted whole grain bread with avocado, hemp seeds, and broccoli sprouts | Blueberries | Green tea Lunch: Quinoa salad with roasted cauliflower, chickpeas, turmeric, walnuts, dried cranberries, and lemon-EVOO dressing Dinner: Lentil Bolognese with tomatoes, garlic, onion, turmeric, and fresh basil on whole grain pasta
Friday Breakfast: Oatmeal with 1 tbsp ground flaxseed, 1 tbsp chia, walnuts, strawberries, cinnamon | Matcha Lunch: Tempeh Buddha bowl — roasted tempeh + brown rice + steamed kale + sesame-ginger dressing + pumpkin seeds Dinner: Moroccan-spiced chickpea stew with preserved lemon, turmeric, ginger, cumin, and leafy greens
Saturday Breakfast: Blueberry-walnut smoothie bowl — blended blueberries + banana + plant milk, topped with granola, hemp seeds, pomegranate, and cacao nibs Lunch: Massaged kale salad with avocado, black beans, tart cherries, walnuts, and tahini-lemon dressing Dinner: Mushroom and lentil shepherd's pie with turmeric mashed sweet potato topping
Sunday Breakfast: Weekend golden milk pancakes (oat flour + turmeric + cinnamon + ground flaxseed) topped with fresh berries and maple syrup | Ginger tea Lunch: Large roasted vegetable and grain bowl with broccoli, Brussels sprouts, sweet potato, and tahini-garlic sauce Dinner: Thai-inspired coconut curry with tofu, bok choy, bell peppers, and jasmine rice | Side of kimchi
Frequently Asked Questions
Can a vegan diet really reduce inflammation as effectively as a Mediterranean diet including fish?
A well-designed vegan diet can match and in some respects exceed the anti-inflammatory effects of a Mediterranean diet including fish — particularly for inflammatory conditions driven by gut microbiome dysbiosis, where the fiber advantage of a whole-food vegan diet is decisive. The primary advantage of Mediterranean diets including fish is the direct EPA+DHA content from seafood, which provides preformed long-chain omega-3s that produce specialized pro-resolving mediators (SPMs). This advantage is fully addressed by algae-based omega-3 supplementation, which provides identical EPA+DHA from the same original source (microalgae) without the animal intermediary. Research published in JAMA Internal Medicine comparing vegan diets to omnivorous diets found that vegans had significantly lower CRP, IL-6, and other inflammatory biomarkers — independent of omega-3 status. The key is ensuring comprehensive nutritional adequacy through strategic supplementation.
What are the most important foods to prioritize on a vegan anti-inflammatory diet?
If forced to identify the five highest-leverage daily priorities: (1) ground flaxseed or chia seeds for ALA omega-3s alongside algae oil supplementation for EPA+DHA; (2) turmeric with black pepper and fat at every savory meal for NF-kB and JAK-STAT inhibition; (3) a diverse array of colorful vegetables and fruits (aiming for 30+ plant varieties weekly) for microbiome-supporting fiber diversity and polyphenol coverage; (4) legumes daily for butyrate-producing resistant starch and complete protein; (5) EVOO as the primary fat for oleocanthal COX inhibition and hydroxytyrosol NF-kB suppression.
How quickly can a vegan anti-inflammatory diet reduce inflammatory markers like CRP?
Clinical research on dietary anti-inflammatory interventions consistently shows measurable CRP and IL-6 reductions within four to eight weeks of implementing a comprehensive whole-food plant-based dietary pattern. The mechanisms with the fastest onset are glucose stabilization (within days — post-meal glucose spikes activate NF-kB immediately), gut microbiome diversity improvement (two to four weeks of consistent high-fiber eating shows measurable microbiome composition changes), and polyphenol NF-kB inhibition (acute effects on inflammatory signaling appear within hours of consumption). Structural changes — improved omega-3 membrane composition, restored B12/homocysteine balance, and optimized vitamin D immune modulation — require weeks to months of consistent implementation.
Is soy anti-inflammatory or inflammatory for vegans?
Whole soy foods — edamame, tempeh, tofu, miso — are anti-inflammatory for most people. Isoflavones in soy (genistein, daidzein) specifically inhibit NF-kB and reduce CRP in multiple clinical trials. Fermented soy products (tempeh, miso, natto) provide additional anti-inflammatory benefits from fermentation-derived bioavailable isoflavones and beneficial bacteria. The concern about soy is largely based on the estrogenic activity of isoflavones in animal studies — human trials consistently show that whole soy consumption does not increase estrogen-related cancer risk and in several studies shows protective effects. Processed soy products (soy protein isolate in protein bars and processed foods) may have different effects and are not equivalent to whole soy foods. For the majority of people, tempeh and tofu are among the most valuable foods in a vegan anti-inflammatory diet.
How do vegans get enough protein for anti-inflammatory enzyme synthesis?
Adequate protein is critical for anti-inflammatory outcomes because glutathione, superoxide dismutase, and all Phase II detoxification enzymes are proteins requiring complete amino acid availability. The myth that vegans cannot get adequate complete protein from plants is nutritionally obsolete. Legumes + grains at any point during the day (not necessarily at the same meal) provide complementary amino acid profiles equivalent to animal protein. Individual complete plant proteins include: quinoa, hemp seeds, chia seeds, soy (edamame, tofu, tempeh), buckwheat, and amaranth. Vegans should target 0.8–1.0g of protein per kg of body weight daily, with emphasis on leucine-rich sources (edamame, tofu, lentils) for muscle protein synthesis. A daily dietary pattern including lentils, tofu or tempeh, hemp seeds, and whole grains provides more than adequate complete protein for anti-inflammatory enzyme synthesis and tissue repair.
What should vegans monitor through blood tests for anti-inflammatory optimization?
Annual blood panel recommendations for vegans focused on anti-inflammatory outcomes: (1) serum vitamin B12 (methylmalonic acid is more sensitive than serum B12 alone); (2) 25(OH)D (vitamin D) — target 40–60 ng/mL; (3) omega-3 index (EPA+DHA as percentage of red blood cell membrane fatty acids) — target above 8%; (4) CRP and/or homocysteine as direct inflammatory markers; (5) ferritin and serum iron for iron status; (6) zinc (serum zinc, though imperfect); (7) TSH and free T4 for thyroid function, as iodine insufficiency affects thyroid-driven inflammatory regulation. These tests together give a comprehensive picture of the nutritional adequacy that determines whether a vegan diet is genuinely anti-inflammatory or merely animal-product-free.
References and Further Reading
Barnard ND et al. — JAMA Internal Medicine (2019) — Plant-based diets and inflammatory markers: systematic review and meta-analysis Meta-analysis of controlled trials demonstrating that plant-based diets significantly reduce CRP, IL-6, and other inflammatory biomarkers compared to omnivorous dietary patterns, with effect sizes comparable to pharmaceutical anti-inflammatory interventions for CRP reduction specifically.
Estruch R et al. — New England Journal of Medicine (PREDIMED Trial, 2013) — Primary Prevention of Cardiovascular Disease with a Mediterranean Diet Landmark randomized trial of 7,447 participants demonstrating that a Mediterranean diet supplemented with EVOO reduced major cardiovascular events by 30% — with inflammatory biomarker reduction, including CRP and IL-6, as primary documented mechanisms supporting the cardiovascular protective effect.
Rogero MM & Calder PC — Nutrients (2018) — Obesity, Inflammation, Toll-Like Receptor 4 and Fatty Acids Comprehensive review of the mechanisms by which dietary fatty acids — including plant-derived ALA and algae-derived EPA/DHA — modulate inflammatory signaling through TLR4, NF-kB, and specialized pro-resolving mediator production, with specific relevance to vegan omega-3 strategy and supplementation guidance.
Sonnenburg JL & Bäckhed F — Nature (2016) — Diet-microbiota interactions as moderators of human metabolism Foundational review establishing the gut microbiome-inflammation axis: how dietary fiber diversity drives microbiome diversity, SCFA production, intestinal barrier function, and systemic inflammatory regulation — with specific evidence for plant-based dietary patterns and their superior microbiome-modulating effects compared to low-fiber omnivorous diets.
About the Author
I'm Judith, a wellness enthusiast and Applied Bio Sciences and Biotechnology graduate behind BiteBrightly. With a deep-rooted belief in the healing power of food, my nutrition journey began with a personal transformation—I improved my eyesight through targeted dietary changes. This life-changing experience sparked my mission to empower others by sharing evidence-based insights into food as medicine.
Drawing on my scientific background, personal experience, and ongoing research into nutrition and health, I focus on breaking down complex health topics into clear, practical, and actionable guidance. My approach combines scientific credibility with real-world application, making evidence-based nutrition accessible to everyone.
Follow me on Pinterest for daily health tips, recipes, and wellness inspiration.
Important Notice: The information in this article is for educational purposes only and is not intended as medical advice. I am not a medical doctor, registered dietitian, or licensed healthcare practitioner. Always consult a qualified healthcare provider before making significant dietary changes, starting supplementation, or modifying any existing medical treatment — particularly if you manage autoimmune conditions, inflammatory diseases, or take medications. Individuals with specific health conditions (thyroid disease, kidney disease, certain autoimmune conditions) may have modified nutritional requirements that differ from the general guidance in this article. Individual results vary based on genetics, health status, gut microbiome composition, and lifestyle factors. These statements have not been evaluated by the FDA.
Connect
Join our newsletter for fresh health tips
© 2026. All rights reserved.