Prediabetes Diet Food List: Reverse It Before It's Diabetes
Reverse prediabetes with this complete food list. 96 million Americans affected. Learn best foods, what to avoid, meal strategies. 58% risk reduction possible.
by BiteBrightly
2/16/202618 min read

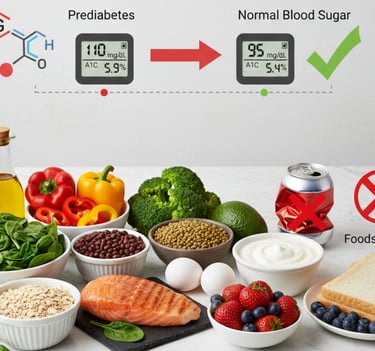
Prediabetes Diet Food List: Reverse It Before It's Diabetes
By BiteBrightly 16 February 2026: This post might contain affiliate links.
Your annual physical comes back with a number that makes your heart sink: fasting blood glucose 110 mg/dL. "You have prediabetes," your doctor says. "Your A1C is 5.9%. If you don't make changes, you'll develop type 2 diabetes within 5-10 years." The diagnosis feels like a ticking time bomb. Your doctor hands you a pamphlet about "eating better and exercising more"—vague advice that leaves you overwhelmed and confused. You know you should change your diet, but what exactly should you eat? What should you avoid? Every article you find contradicts the last one. Low-carb? Low-fat? Mediterranean? Keto? You're paralyzed by information overload while your blood sugar continues creeping upward. What if there's a clear, evidence-based food list that can actually reverse prediabetes before it becomes full diabetes? What if specific foods—not generic advice to "eat healthy"—could lower your blood sugar, improve insulin sensitivity, and give you a realistic chance of avoiding diabetes entirely? If you're searching for a prediabetes diet food list that actually works, backed by science and proven to reverse progression, you're about to discover that prediabetes isn't a life sentence—it's a powerful wake-up call with a clear nutritional solution.
Prediabetes affects approximately 96 million American adults—more than 1 in 3 people. According to research from the CDC, more than 80% of people with prediabetes don't know they have it. Without intervention, 15-30% of people with prediabetes will develop type 2 diabetes within 5 years. However—and this is crucial—prediabetes is reversible. According to the landmark Diabetes Prevention Program study, lifestyle interventions including dietary changes reduced diabetes risk by 58% (71% in people over 60).
The connection between diet and blood sugar is direct and immediate. Every food you eat affects your blood glucose levels. Simple carbohydrates (white bread, sugary drinks, pastries) cause rapid blood sugar spikes. Refined carbs without fiber are absorbed quickly, flooding your bloodstream with glucose. Your pancreas responds by releasing insulin to shuttle glucose into cells. Over time, cells become resistant to insulin's signals—this is insulin resistance, the hallmark of prediabetes. Your pancreas compensates by producing more insulin, but eventually can't keep up. Blood sugar stays elevated, and prediabetes progresses to type 2 diabetes.
Here's what most people don't understand about prediabetes: it's not just about avoiding sugar. It's about choosing foods that stabilize blood sugar, improve insulin sensitivity, reduce inflammation, and support healthy metabolism. Fiber-rich whole grains slow glucose absorption. Protein and healthy fats blunt blood sugar spikes. Non-starchy vegetables provide volume and nutrients without raising blood sugar. Specific foods contain compounds that enhance insulin sensitivity and glucose metabolism. Strategic meal composition—combining protein, fiber, and healthy fats—prevents the blood sugar rollercoaster that drives diabetes progression.
According to research in The Lancet, dietary interventions targeting blood sugar control are among the most effective strategies for diabetes prevention. Weight loss of just 5-7% body weight (for a 200-pound person, that's 10-14 pounds) combined with dietary changes can reduce diabetes risk by over 50%. You don't need to be perfect—you need to be strategic and consistent.
This comprehensive guide reveals the best foods for prediabetes (organized by category for easy reference), why each food helps reverse insulin resistance and lower blood sugar, foods to avoid or limit (the blood sugar saboteurs), realistic meal composition strategies (not just lists—actual eating patterns), sample prediabetes-reversal days showing exactly what to eat, and how quickly you can expect blood sugar improvements with dietary changes.
Key Takeaways
96 million Americans have prediabetes; 80%+ don't know it
Prediabetes is reversible—lifestyle intervention reduces diabetes risk by 58%
Prediabetes defined: fasting glucose 100-125 mg/dL OR A1C 5.7-6.4%
Key strategy: Stabilize blood sugar through fiber, protein, healthy fats, and low-glycemic carbs
Best foods: Non-starchy vegetables, legumes, whole grains, lean proteins, healthy fats, berries
Worst foods: Sugary drinks, refined carbs, white bread/rice/pasta, processed foods, excess fruit juice
Meal composition matters: Combine protein + fiber + healthy fat to prevent blood sugar spikes
Portion control critical: Even healthy carbs raise blood sugar if portions are excessive
Timeline: Blood sugar improvements visible in 2-4 weeks; A1C improvements in 2-3 months
Goal: Reverse prediabetes to normal (fasting glucose <100 mg/dL, A1C <5.7%)
Understanding Prediabetes and Blood Sugar
What is Prediabetes?
Prediabetes is a condition where blood sugar levels are higher than normal but not yet high enough to be classified as type 2 diabetes.
Diagnostic criteria (any one of the following):
Fasting blood glucose:
Normal: <100 mg/dL
Prediabetes: 100-125 mg/dL
Diabetes: ≥126 mg/dL
A1C (average blood sugar over 2-3 months):
Normal: <5.7%
Prediabetes: 5.7-6.4%
Diabetes: ≥6.5%
Oral glucose tolerance test (2-hour value):
Normal: <140 mg/dL
Prediabetes: 140-199 mg/dL
Diabetes: ≥200 mg/dL
What Causes Prediabetes?
Insulin resistance: The primary driver. Your cells become less responsive to insulin's signal to absorb glucose from the bloodstream. Your pancreas compensates by producing more insulin (hyperinsulinemia), but eventually can't keep up. Blood sugar rises.
Contributing factors:
Excess body weight (especially abdominal fat)
Physical inactivity
Poor diet (high in refined carbs, sugar, processed foods)
Genetics and family history
Age (risk increases after 45)
Gestational diabetes history
Polycystic ovary syndrome (PCOS)
Sleep disorders (sleep apnea)
Chronic stress
Why Diet Matters So Much
Diet directly impacts blood sugar and insulin sensitivity:
Foods that spike blood sugar:
Refined carbohydrates (white bread, white rice, pastries)
Sugary foods and beverages
Low-fiber, high-glycemic foods
Foods that stabilize blood sugar:
High-fiber foods (slow glucose absorption)
Protein (minimal blood sugar impact, increases satiety)
Healthy fats (slow digestion, prevent spikes)
Low-glycemic carbohydrates
Meal composition matters: Combining protein, fiber, and fat with carbohydrates dramatically reduces blood sugar response compared to eating carbs alone.
The Goal: Reverse Prediabetes
Target blood sugar levels:
Fasting glucose: <100 mg/dL (ideally 70-90 mg/dL)
A1C: <5.7% (ideally <5.5%)
Post-meal glucose (1-2 hours after eating): <140 mg/dL
How to achieve it:
Strategic food choices (this guide)
Weight loss (5-7% if overweight)
Regular physical activity (150 min/week moderate exercise)
Adequate sleep (7-9 hours)
Stress management
Best Foods for Prediabetes (Eat Freely/Regularly)
Category 1: Non-Starchy Vegetables (Unlimited)
Non-starchy vegetables have minimal impact on blood sugar and should form the foundation of a prediabetes diet.
Why they're essential:
Very low in carbohydrates and calories
High in fiber (slows glucose absorption)
Packed with vitamins, minerals, and antioxidants
High volume for satiety without blood sugar impact
Best choices:
Leafy greens: Spinach, kale, lettuce, arugula, Swiss chard, collard greens
Cruciferous: Broccoli, cauliflower, Brussels sprouts, cabbage
Other: Bell peppers, cucumbers, zucchini, asparagus, green beans, celery, mushrooms, tomatoes, onions, garlic
How to use: Fill half your plate with non-starchy vegetables at lunch and dinner. Use as snacks (bell pepper strips, cucumber slices, cherry tomatoes).
Category 2: Legumes and Beans (Regularly, Portion-Controlled)
Beans and lentils are excellent for blood sugar control despite containing carbohydrates.
Why they work:
High in fiber (15-16g per cup!)
Low glycemic index (slow, gradual blood sugar rise)
High in protein (supports satiety, minimal blood sugar impact)
Resistant starch (feeds beneficial gut bacteria, improves insulin sensitivity)
Best choices:
Lentils (all varieties: green, red, brown)
Black beans
Kidney beans
Chickpeas
Navy beans
Pinto beans
How to use: 1/2 to 1 cup per meal, 4-5 times weekly. Combine with non-starchy vegetables and lean protein. Make lentil soup, bean salads, chickpea curry.
Blood sugar tip: Pair beans with vinegar (in salad dressing) or lemon juice—acetic acid further blunts blood sugar response.
Category 3: Whole Grains (Moderate Portions, Strategic Use)
Whole grains are better than refined grains but still contain carbohydrates requiring portion control.
Why they're better than refined:
Intact fiber slows digestion and glucose absorption
Vitamins, minerals, and phytonutrients
More satisfying than refined grains
Best choices (lower glycemic):
Steel-cut oats or rolled oats (not instant)
Quinoa
Barley
Bulgur
Farro
Brown rice (lower GI than white rice)
Wild rice
Whole grain bread (truly whole grain, 3g+ fiber per slice)
Portions:
1/2 cup cooked grains per meal (not 1-2 cups!)
1-2 slices whole grain bread (not 3-4)
How to use: Combine with protein, healthy fat, and vegetables. Example: 1/2 cup quinoa + grilled chicken + large salad + olive oil dressing.
Avoid: White rice, white bread, white pasta, instant oatmeal with added sugar.
Category 4: Lean Proteins (Regularly, Every Meal)
Protein has minimal impact on blood sugar and is crucial for satiety and muscle maintenance.
Why protein helps:
Minimal blood sugar impact (unlike carbs)
Increases satiety (prevents overeating)
Supports muscle mass (important for insulin sensitivity)
Slows digestion when combined with carbs
Best choices:
Skinless poultry: Chicken breast, turkey
Fish: Salmon, tuna, cod, sardines, mackerel (omega-3s improve insulin sensitivity)
Eggs (whole eggs—yolks contain nutrients)
Greek yogurt (plain, unsweetened—high protein, low sugar)
Tofu and tempeh
Cottage cheese (low-fat or full-fat, unsweetened)
Lean beef or pork (moderate amounts)
How to use: Include 3-4 oz (palm-sized portion) at each meal. Pair with non-starchy vegetables and moderate carbs.
Category 5: Healthy Fats (Moderate Amounts, Daily)
Healthy fats don't raise blood sugar and help prevent spikes when eaten with carbs.
Why they help:
Zero blood sugar impact
Slow digestion (blunt blood sugar response to carbs)
Support satiety (prevent overeating)
Anti-inflammatory (reduce inflammation linked to insulin resistance)
Best choices:
Avocado (1/4 to 1/2 per meal)
Nuts: Almonds, walnuts, pecans, cashews (1 oz/small handful)
Seeds: Chia, flax, pumpkin, hemp
Olive oil (extra virgin—1-2 tablespoons for cooking/dressing)
Fatty fish (salmon, mackerel, sardines—omega-3s)
Nut butters (natural, no added sugar—1-2 tablespoons)
Avoid: Trans fats (partially hydrogenated oils), excessive saturated fats (deep-fried foods, fatty cuts of meat).
Category 6: Berries and Low-Glycemic Fruits (Moderate Portions)
Most fruits contain sugar, but berries and some other fruits have lower glycemic impact.
Best choices:
Berries: Strawberries, blueberries, raspberries, blackberries (1/2 to 1 cup)
Cherries (1/2 cup)
Apples (1 small, with skin for fiber)
Pears (1 small, with skin)
Grapefruit (1/2)
Oranges (1 small)
Portions: 1/2 to 1 cup berries OR 1 small piece of fruit per meal or snack.
How to use: Pair with protein or fat (berries + Greek yogurt, apple + almond butter) to further blunt blood sugar response.
Limit/Avoid: Fruit juice (even 100% juice—no fiber, rapid blood sugar spike), dried fruit (concentrated sugar), tropical fruits in large amounts (pineapple, mango, banana—higher glycemic).
Category 7: Nuts and Seeds (Daily Snacks, Portion-Controlled)
Nuts and seeds are low-carb, high-fiber, high-fat foods excellent for blood sugar control.
Why they help:
Low glycemic impact
High in fiber and protein
Healthy fats slow digestion
Magnesium (improves insulin sensitivity)
Best choices:
Almonds (1 oz = 23 almonds)
Walnuts (1 oz = 14 halves)
Pistachios (1 oz = 49 nuts)
Pecans, macadamia nuts, Brazil nuts
Chia seeds (1-2 tablespoons)
Flaxseeds (ground, 1-2 tablespoons)
Pumpkin seeds
Portions: 1 oz (small handful) per snack, 1-2 times daily.
Blood sugar tip: Studies show almonds and walnuts specifically improve blood sugar control and insulin sensitivity when consumed regularly.
Category 8: Fermented Foods (Gut Health = Metabolic Health)
Emerging research links gut health to insulin sensitivity and blood sugar control.
Why they help:
Probiotics improve gut microbiome
May enhance insulin sensitivity
Best choices:
Plain Greek yogurt (unsweetened)
Kefir (unsweetened)
Sauerkraut
Kimchi
Tempeh
Miso
Kombucha (unsweetened or low-sugar)
How to use: 1 serving daily. Greek yogurt for breakfast, kimchi or sauerkraut as side dish.
Category 9: Herbs, Spices, and Specific Foods with Blood Sugar Benefits
Certain foods contain compounds that may improve insulin sensitivity or glucose metabolism.
Cinnamon: May improve insulin sensitivity. Add 1/2 to 1 teaspoon daily to oatmeal, yogurt, coffee.
Apple cider vinegar: Acetic acid blunts blood sugar response. Use 1-2 tablespoons in salad dressing or diluted in water before meals.
Turmeric (curcumin): Anti-inflammatory, may improve insulin sensitivity. Use in cooking, golden milk.
Ginger: May improve fasting blood sugar. Use fresh or powdered in cooking, tea.
Garlic: May improve blood sugar and insulin sensitivity. Use fresh in cooking.
Green tea: Catechins may improve insulin sensitivity. Drink 2-3 cups daily.
Foods to Avoid or Strictly Limit
Category 1: Sugary Beverages (Avoid Completely)
The worst offenders for blood sugar.
Avoid:
Regular soda (35-40g sugar per 12 oz can—massive spike)
Fruit juice (even 100% juice—no fiber, rapid absorption)
Sweet tea (sweetened)
Energy drinks (loaded with sugar)
Specialty coffee drinks (frappuccinos, mochas with syrups)
Sports drinks (unless exercising intensely)
Why they're terrible: Liquid sugar absorbed extremely rapidly, causing sharp blood sugar spike with no satiety. Regular consumption strongly linked to type 2 diabetes.
Alternatives: Water, sparkling water, unsweetened tea, coffee (black or with small amount of milk/cream), water with lemon/cucumber.
Category 2: Refined Grains (Minimize or Avoid)
Stripped of fiber, refined grains act like sugar in your body.
Avoid/Minimize:
White bread
White rice
White pasta
Bagels, donuts, pastries
Most crackers
Pretzels
Instant oatmeal with added sugar
Most breakfast cereals (high sugar, low fiber)
Why they're problematic: Refined grains are rapidly digested and absorbed, causing blood sugar spikes similar to eating pure sugar.
Better alternatives: Whole grain versions in SMALL portions (1/2 cup cooked), or replace with non-starchy vegetables.
Category 3: Sweets and Desserts (Occasional Treats Only)
Obvious blood sugar saboteurs.
Minimize:
Candy
Cookies, cakes, pies
Ice cream
Pastries
Sweetened yogurt (6-20g added sugar!)
Strategy: If you eat dessert, do so occasionally, in small portions, immediately after a balanced meal (not on empty stomach). The protein and fiber from the meal will slightly blunt the blood sugar spike.
Better alternative: Berries with Greek yogurt, dark chocolate (70%+ cocoa, 1 oz).
Category 4: Processed and Packaged Foods (Read Labels!)
Many processed foods contain hidden sugars and refined carbs.
Watch out for:
Breakfast cereals (most have 10-20g sugar per serving)
Granola bars (often 10-15g sugar)
Flavored yogurt (12-20g added sugar)
Jarred pasta sauce (added sugar)
Condiments (ketchup, BBQ sauce—loaded with sugar)
"Low-fat" products (often high in added sugar)
Strategy: Read nutrition labels. Look for <5g sugar per serving, 3g+ fiber. Ingredient list should be short and recognizable.
Category 5: Certain Fruits in Excess
While fruit has fiber and nutrients, high-sugar fruits can raise blood sugar significantly.
Limit:
Bananas (especially ripe ones—higher glycemic)
Grapes (very high sugar concentration)
Pineapple (higher glycemic)
Mango (higher sugar)
Watermelon (higher glycemic despite being mostly water)
Dried fruit (concentrated sugar, easy to overeat)
ALL fruit juice
Strategy: Stick to berries and lower-glycemic fruits (see "Best Foods" section). Limit to 1-2 servings daily, always paired with protein or fat.
Category 6: Alcohol (Moderate Carefully)
Alcohol affects blood sugar unpredictably.
Issues:
Can cause blood sugar spikes (beer, sweet cocktails)
Can cause blood sugar drops (especially on empty stomach)
Impairs judgment (leads to poor food choices)
High in empty calories
If you drink:
Limit to 1 drink for women, 2 for men daily
Choose lower-carb options (dry wine, light beer, spirits with zero-calorie mixer)
Never drink on empty stomach (eat protein/fat with alcohol)
Monitor blood sugar if diabetic or on medication
Strategic Meal Composition: The Prediabetes Plate
Understanding what to eat is only half the battle. HOW you combine foods determines blood sugar response.
The Prediabetes Plate Method
50% Non-Starchy Vegetables:
Fill half your plate with vegetables (spinach, broccoli, cauliflower, bell peppers, salad, etc.)
Provides volume, fiber, nutrients without blood sugar impact
25% Lean Protein:
Palm-sized portion (3-4 oz)
Chicken, fish, tofu, eggs, Greek yogurt
Stabilizes blood sugar, supports satiety
25% Healthy Carbohydrates:
1/2 cup cooked whole grains OR 1 cup legumes/beans
Choose lower-glycemic options
Portion control is CRITICAL
Add Healthy Fat:
1-2 tablespoons olive oil (dressing, cooking)
OR 1/4 avocado
OR small handful nuts
Example Meal:
2 cups mixed greens salad with tomatoes and cucumbers (non-starchy veg)
4 oz grilled salmon (protein + healthy fat)
1/2 cup quinoa (healthy carb)
Olive oil + lemon dressing (healthy fat)
Snack Strategy
Smart snacks (blood sugar-friendly):
Greek yogurt (plain) + berries
Apple + almond butter (1-2 tablespoons)
Vegetables + hummus
Hard-boiled eggs
Small handful almonds or walnuts
Cottage cheese + cucumber slices
String cheese + bell pepper strips
Avoid:
Crackers, chips, pretzels alone (refined carbs without protein/fat)
Granola bars (usually high sugar)
Dried fruit alone
Candy, cookies
Sample Prediabetes-Reversal Days
Sample Day 1: Omnivore
Breakfast (7:00 AM):
2 scrambled eggs (protein)
1/2 cup steel-cut oats (fiber-rich carb)
1/2 cup blueberries (low-glycemic fruit)
1 tablespoon ground flaxseed (healthy fat, fiber)
Cinnamon (blood sugar benefit)
Black coffee or unsweetened tea
Mid-Morning Snack (10:00 AM):
1 small apple + 1 tablespoon almond butter
Lunch (12:30 PM):
Large salad: 2-3 cups mixed greens, tomatoes, cucumbers, bell peppers
4 oz grilled chicken breast
1/2 cup chickpeas
Olive oil + vinegar dressing (2 tablespoons)
Water with lemon
Afternoon Snack (3:30 PM):
1/4 cup hummus + raw vegetables (carrots, bell peppers, cucumber)
Dinner (6:30 PM):
4-5 oz baked salmon
1-1.5 cups roasted broccoli and cauliflower (olive oil, garlic)
1/2 cup brown rice
Side salad with olive oil dressing
Evening (if hungry):
1 oz almonds OR plain Greek yogurt (1/2 cup)
Daily totals (approximate):
Carbohydrates: 120-150g (from whole grains, legumes, vegetables, fruit)
Protein: 100-120g
Fiber: 35-45g
Healthy fats: adequate
Blood sugar impact: Stable throughout day, no sharp spikes.
Sample Day 2: Vegetarian
Breakfast:
Plain Greek yogurt (1 cup)
1/2 cup strawberries
2 tablespoons chia seeds
1/4 cup walnuts
Cinnamon
1/4 avocado on 1 slice whole grain toast
Lunch:
Lentil soup (1.5 cups—high fiber, protein)
Large side salad with olive oil dressing
1 small whole grain roll (if desired)
Snack:
Celery sticks + 2 tablespoons natural peanut butter
Dinner:
Tofu stir-fry: 6 oz firm tofu, 2-3 cups mixed vegetables (broccoli, bell peppers, snap peas, mushrooms), garlic, ginger
1/2 cup quinoa
Cooked in 1 tablespoon olive oil
Evening:
Herbal tea + 5-6 almonds
Daily totals: Similar to Day 1—controlled carbs, high fiber, adequate protein and healthy fats.
Timeline: When Will You See Results?
Week 1-2: Initial blood sugar improvements. Fasting glucose may drop 5-15 mg/dL. Reduced post-meal spikes.
Week 2-4: Continued improvements. Better energy, less hunger. Fasting glucose stabilizing.
Month 2-3: A1C improvements visible (if retested). A1C may drop 0.2-0.5%. Weight loss if overweight (supporting further improvement).
Month 3-6: Significant progress. Many people reverse prediabetes to normal blood sugar ranges (fasting <100 mg/dL, A1C <5.7%) with consistent dietary changes + weight loss + exercise.
Long-term: Sustained reversal requires ongoing healthy eating patterns. Prediabetes can return if old habits resume.
Additional Strategies Beyond Food Choices
Portion Control
Even healthy carbs raise blood sugar if portions are excessive.
Key portions:
Cooked whole grains: 1/2 cup (not 1-2 cups)
Legumes/beans: 1/2 to 1 cup
Fruit: 1/2 to 1 cup berries OR 1 small piece
Starchy vegetables (sweet potato): 1/2 cup or 1 small
Strategy: Use measuring cups initially to recalibrate portion sizes. Most people underestimate portions significantly.
Meal Timing and Frequency
Consistent meal timing: Eating at regular times helps regulate blood sugar.
Don't skip meals: Skipping meals often leads to overeating later and blood sugar instability.
Stop eating 2-3 hours before bed: Allows blood sugar to normalize overnight.
Physical Activity
Exercise improves insulin sensitivity independently of diet.
Target: 150 minutes/week moderate activity (brisk walking, cycling, swimming).
Post-meal walks: A 15-20 minute walk after meals significantly reduces post-meal blood sugar spikes.
Weight Loss (If Overweight)
Losing 5-7% of body weight dramatically improves insulin sensitivity and blood sugar control.
For 200-pound person: That's just 10-14 pounds!
How dietary changes help: The prediabetes diet naturally supports weight loss (high fiber, high protein, controlled portions).
Monitor Blood Sugar
Home glucose meter: Check fasting glucose weekly. Check 1-2 hours after meals occasionally to see how foods affect you.
Target post-meal: <140 mg/dL at 1-2 hours after eating.
A1C testing: Retest A1C every 2-3 months to track progress.
Stress Management and Sleep
Chronic stress: Elevates cortisol, which raises blood sugar and worsens insulin resistance.
Poor sleep: Impairs insulin sensitivity and increases cravings for high-carb foods.
Solutions: Prioritize 7-9 hours sleep, practice stress reduction (meditation, yoga, deep breathing).
Special Considerations
Prediabetes During Pregnancy
Gestational diabetes increases future type 2 diabetes risk.
Strategy: Work closely with healthcare provider. Dietary changes similar to prediabetes diet but with appropriate calorie and nutrient intake for pregnancy.
Prediabetes with Other Conditions
PCOS: Often linked to insulin resistance. Prediabetes diet aligns well with PCOS management.
High cholesterol/heart disease: Prediabetes diet supports cardiovascular health (high fiber, healthy fats, lean protein).
Medications
Some people need metformin (medication) in addition to lifestyle changes.
Metformin: Can be prescribed for prediabetes, especially if high risk or not responding to lifestyle alone.
Never replace medication with diet without doctor approval. Diet and medication work together.
Conclusion
Prediabetes isn't a death sentence—it's a wake-up call. A powerful opportunity to reverse course before full diabetes develops. The diagnosis can feel overwhelming, but the solution is clearer than you might think: strategic food choices that stabilize blood sugar, improve insulin sensitivity, reduce inflammation, and support healthy metabolism.
The prediabetes diet isn't about deprivation or bland "diabetic food." It's about abundance of the RIGHT foods. Fill your plate with non-starchy vegetables (unlimited). Build meals around lean protein (every meal). Choose fiber-rich whole grains and legumes in moderate portions. Include healthy fats that slow digestion and prevent blood sugar spikes. Enjoy berries and low-glycemic fruits. Embrace nuts, seeds, and fermented foods.
Avoid the blood sugar saboteurs: sugary beverages (the worst!), refined grains (white bread, white rice, white pasta), sweets and processed foods, excessive fruit and fruit juice. These aren't occasional indulgences when you have prediabetes—they're actively driving progression toward diabetes.
Master meal composition: The 50% vegetables, 25% protein, 25% healthy carbs plate method ensures balanced meals that won't spike blood sugar. Pair carbs with protein and fat. Control portions even of healthy foods. Eat at regular times. Stay active. Lose 5-7% body weight if overweight.
Monitor your progress. Check fasting glucose weekly with a home meter. Retest A1C every 2-3 months. Most people see fasting glucose drop 5-15 mg/dL within 2-4 weeks. A1C improvements visible in 2-3 months. Many people reverse prediabetes to normal blood sugar ranges (fasting <100 mg/dL, A1C <5.7%) within 3-6 months of consistent dietary changes combined with weight loss and exercise.
The Diabetes Prevention Program proved lifestyle intervention reduces diabetes risk by 58%. You're not powerless. You have agency. Every meal is a choice. Every day is an opportunity to stabilize blood sugar, improve insulin sensitivity, and move away from diabetes rather than toward it.
Prediabetes reversed isn't just a number on a lab report. It's sustained energy throughout the day without blood sugar crashes. It's freedom from the fear of diabetes complications—blindness, amputation, kidney failure, heart disease. It's taking control of your health through evidence-based nutrition.
Your blood sugar is elevated, but it's not diabetes yet. You're standing at a crossroads. One path leads to progression, medications, complications. The other path—the one illuminated by this food list and these strategies—leads to reversal, health, and vitality.
Choose the path of reversal. Start today.
To normal blood sugar, vibrant health, and a diabetes-free future!
References and Further Reading
Centers for Disease Control and Prevention - Prediabetes: Your Chance to Prevent Type 2 Diabetes
Diabetes Prevention Program Research Group - Reduction in Diabetes Incidence (NEJM)
American Diabetes Association - Standards of Medical Care in Diabetes
Frequently Asked Questions
Can prediabetes really be reversed or is it permanent?
Yes, prediabetes is REVERSIBLE! The landmark Diabetes Prevention Program study showed lifestyle intervention (diet + exercise + modest weight loss) reduced diabetes risk by 58%. Many people successfully reverse prediabetes to normal blood sugar levels (fasting glucose <100 mg/dL, A1C <5.7%) within 3-6 months of consistent dietary changes. However, reversal requires ongoing healthy habits—if you return to old eating patterns, prediabetes can return. The key is making sustainable changes you can maintain long-term, not temporary diets.
What are the best foods to eat if I have prediabetes?
Focus on: Non-starchy vegetables (unlimited—spinach, broccoli, cauliflower, peppers, salad greens), legumes and beans (lentils, chickpeas, black beans—1/2 to 1 cup per meal), lean proteins (chicken, fish, eggs, Greek yogurt, tofu—every meal), whole grains in moderate portions (1/2 cup quinoa, oats, brown rice), healthy fats (avocado, nuts, olive oil, fatty fish), and berries/low-glycemic fruits (1/2 to 1 cup). These foods stabilize blood sugar, improve insulin sensitivity, and provide satiety without blood sugar spikes.
What foods should I completely avoid with prediabetes?
Eliminate or strictly limit: Sugary beverages (soda, juice, sweet tea—the worst offenders), refined grains (white bread, white rice, white pasta, pastries), sweets and desserts (candy, cookies, ice cream), processed foods with added sugars, and excessive fruit juice (even 100% juice has no fiber and spikes blood sugar). These foods cause rapid blood sugar spikes and worsen insulin resistance. Focus on whole, unprocessed foods instead.
How many carbs should I eat daily with prediabetes?
There's no one-size-fits-all number, but most people with prediabetes do well with 120-150g carbohydrates daily (spread across meals). This is moderate-carb, not extreme low-carb. More important than total carbs is QUALITY and PAIRING: Choose fiber-rich carbs (whole grains, legumes, vegetables) in controlled portions (1/2 cup grains per meal, not 1-2 cups), and always pair carbs with protein and healthy fat to blunt blood sugar response. Monitor your individual response with a glucose meter—some people need fewer carbs, others can tolerate more.
Can I eat fruit if I have prediabetes?
Yes, but choose wisely and control portions. Best fruits: Berries (strawberries, blueberries, raspberries, blackberries—1/2 to 1 cup), cherries, apples, pears, grapefruit, oranges (all in moderation—1 small piece). Limit higher-sugar fruits like bananas, grapes, pineapple, mango, watermelon. AVOID fruit juice completely (no fiber, rapid blood sugar spike). Always pair fruit with protein or fat (berries + Greek yogurt, apple + almond butter) to further stabilize blood sugar response.
How long before I see blood sugar improvements with dietary changes?
Timeline varies by consistency and individual factors, but most people see: Week 1-2: Initial improvements (fasting glucose drops 5-15 mg/dL, reduced post-meal spikes), Week 2-4: Continued improvement and stabilization, Month 2-3: A1C improvements visible if retested (may drop 0.2-0.5% or more), Month 3-6: Significant progress, many reverse to normal blood sugar ranges with consistent changes + weight loss + exercise. Track progress with home glucose meter (fasting weekly, occasional post-meal checks) and A1C testing every 2-3 months.
Is the prediabetes diet the same as the keto diet?
No. The prediabetes diet is moderate-carb (120-150g daily from fiber-rich sources), not very low-carb like keto (20-50g). Prediabetes diet includes whole grains (1/2 cup portions), legumes, fruits (in moderation), and emphasizes vegetables, lean protein, and healthy fats. It's sustainable long-term and supported by extensive research (Diabetes Prevention Program). Keto can work for some but is more restrictive and harder to sustain. Both control blood sugar, but prediabetes diet is more flexible and realistic for most people.
Can I reverse prediabetes without losing weight?
Dietary changes alone improve blood sugar and insulin sensitivity even without weight loss—choosing fiber-rich carbs, pairing meals properly, avoiding refined carbs and sugar all help. However, weight loss amplifies benefits dramatically. Losing just 5-7% body weight (10-14 pounds for a 200-pound person) improves insulin sensitivity independent of diet quality. The prediabetes diet naturally supports weight loss (high fiber, high protein, controlled portions), so many people lose weight even without explicitly trying. For best results, combine dietary changes with modest weight loss.
Should I check my blood sugar at home and how often?
Yes! Home glucose monitoring provides immediate feedback on how foods affect your blood sugar. Get an inexpensive glucose meter and test strips. Check fasting glucose weekly (first thing in morning before eating—target <100 mg/dL, ideally 70-90 mg/dL). Occasionally check 1-2 hours after meals to see blood sugar response (target <140 mg/dL). This helps you identify which foods spike your blood sugar and confirms your dietary changes are working. Also get A1C tested every 2-3 months through your doctor to track overall progress.
Can I drink coffee and alcohol with prediabetes?
Coffee: Yes! Plain black coffee or coffee with small amount of milk/cream is fine. Coffee may even improve insulin sensitivity. Avoid sugar and flavored syrups. Limit specialty drinks (frappuccinos, mochas) loaded with sugar. Alcohol: Moderate carefully. Limit to 1 drink (women) or 2 drinks (men) daily maximum. Choose lower-carb options (dry wine, light beer, spirits with zero-calorie mixer). Never drink on empty stomach (alcohol can cause blood sugar drops). Eat protein/fat with alcohol. Many people find eliminating or minimizing alcohol supports better blood sugar control and weight loss.
About Author
I'm Judith, a wellness enthusiast and Applied Bio Sciences and Biotechnology graduate behind BiteBrightly. With a deep-rooted belief in the healing power of food, my nutrition journey began with a personal transformation—I improved my eyesight through targeted dietary changes. This life-changing experience sparked my mission to empower others by sharing evidence-based insights into food as medicine.
Drawing on my scientific background, personal experience, and ongoing research into nutrition and health, I focus on breaking down complex health topics into clear, practical, and actionable guidance. My approach combines scientific credibility with real-world application, making evidence-based nutrition accessible to everyone.
Follow me on Pinterest for daily health tips, recipes, and wellness inspiration.
Important Notice: The information in this article is for educational purposes only and is not intended as medical advice or to replace professional medical treatment. Always consult your healthcare provider before making dietary changes or implementing health recommendations, especially if you have prediabetes, diabetes, or other medical conditions, or take medications. Blood sugar management requires medical supervision. Get appropriate testing (fasting glucose, A1C, oral glucose tolerance test) to confirm prediabetes diagnosis and monitor progress. Individual responses to dietary changes vary. This information is not intended to replace prescribed medications or medical treatment plans. Work with your healthcare team to develop a comprehensive prediabetes reversal strategy.
Connect
Join our newsletter for fresh health tips
© 2026. All rights reserved.