Zinc-Rich Foods for Acne: Clear Skin From Within
Zinc beats tetracycline in RCTs. Oysters: 670% daily zinc. 5-alpha reductase inhibition. 15 foods, acne science, GI-hormonal connection. Clear skin from within.
by BiteBrightly
3/14/202628 min read
Zinc-Rich Foods for Acne: Clear Skin From Within
By BiteBrightly 13 March 2026: This post might contain affiliate links.
You have tried the topical route. The benzoyl peroxide, the salicylic acid washes, the retinol serums, the niacinamide, the tea tree oil. Maybe prescription antibiotics that worked for a while and then stopped. You cleanse twice daily, change your pillowcase weekly, never touch your face, and still — breakouts arrive on their own schedule, seemingly indifferent to everything you apply to the surface. The frustration is particular: doing everything right and still watching new pimples form in the mirror.
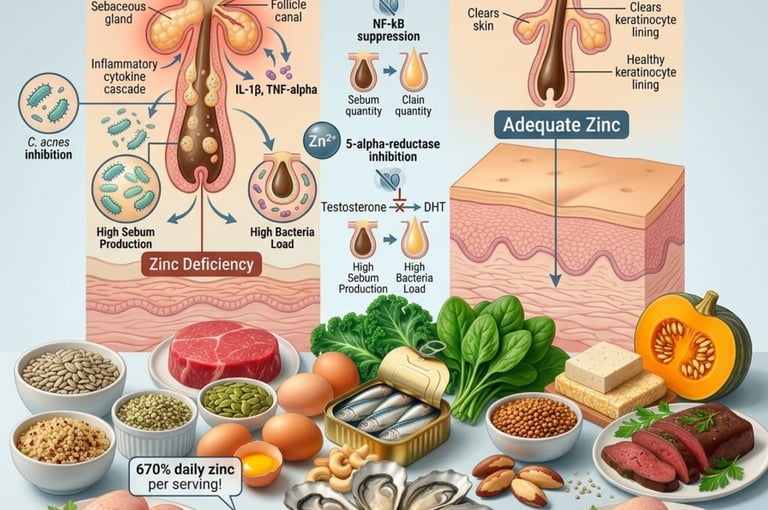
What dermatological skin care rarely addresses is the biology happening beneath the surface — the internal nutritional and hormonal environment that determines whether your skin produces excess sebum, whether your pores become inflamed, whether bacteria proliferate, and whether your immune system mounts a disproportionate inflammatory response to normal skin microbiome inhabitants. Acne is not a surface disease. It is a systemic condition with four simultaneous drivers: excess sebum production, abnormal follicular keratinization, Cutibacterium acnes proliferation, and inflammatory immune response. And all four of these drivers are directly influenced by nutritional status.
Zinc is the mineral at the intersection of all of them. It regulates sebaceous gland activity, modulates the inflammatory cascade that turns a blocked pore into a painful cyst, inhibits the bacterial proliferation that drives pustule formation, normalizes keratinocyte differentiation in the follicle lining, and acts as a required cofactor for the retinoid-binding proteins that make vitamin A skin-clearing work. Multiple randomized controlled trials have directly compared oral zinc supplementation to oral antibiotics for acne — and zinc has performed comparably to tetracycline in several of these trials, without the antibiotic resistance implications, gut microbiome disruption, or photosensitivity side effects.
And yet most skin care conversations never mention zinc. Most dermatological dietary advice, when offered at all, focuses on glycemic index and dairy — important but incomplete. Zinc status, which is suboptimal in a meaningful proportion of acne patients and in the general population more broadly, is the nutritional variable most directly and specifically linked to acne severity in the peer-reviewed literature.
This guide covers the science of zinc and skin health in depth, the fifteen most zinc-dense whole foods you can prioritize for clearer skin, the other nutritional factors that work synergistically with zinc in acne management, and the complete dietary strategy for building a skin-clearing nutritional foundation from within.
Key Takeaways
Zinc is lower in acne patients than in clear-skinned controls in multiple studies — establishing zinc deficiency as a genuine acne risk factor, not just a correlation
Zinc inhibits 5-alpha-reductase, the enzyme that converts testosterone to dihydrotestosterone (DHT) — the androgen that directly stimulates sebaceous gland activity and excess sebum production
Zinc supplementation reduced acne lesion counts comparably to tetracycline (a standard oral antibiotic) in randomized controlled trials, without antibiotic resistance or gut microbiome disruption
Oysters are the single most zinc-dense food available — one serving provides 74mg of zinc, over 670% of the daily recommended intake
Non-heme zinc from plant foods is significantly less bioavailable than zinc from animal sources — vegans and vegetarians need 50% higher zinc intake targets and should prioritize phytate-reduction strategies
Zinc works synergistically with vitamin A (required for retinoid-binding protein synthesis), selenium (antioxidant quenching of inflammatory reactive oxygen species in skin), and omega-3 fatty acids (reducing prostaglandin-driven sebaceous gland stimulation)
The glycemic index–acne connection is mechanistically distinct from and additive to zinc's effects: high-GI diets raise IGF-1 and insulin, both of which activate sebaceous gland androgen receptors independently of DHT
The Biology of Acne: What's Actually Happening in Your Skin
Before examining zinc's specific mechanisms, understanding the four-driver model of acne development explains why a single mineral can have such broad and clinically significant effects.
The Four Drivers of Acne Formation
Driver 1 — Excess sebum production: Sebaceous glands produce sebum (skin oil) under the primary stimulation of androgens — specifically dihydrotestosterone (DHT), which is converted from testosterone by the enzyme 5-alpha-reductase within the sebaceous gland itself. Excess sebum production fills the follicular canal, creating the comedone (blocked pore) that is the precursor to all acne lesions. Zinc inhibits 5-alpha-reductase activity, directly reducing the androgenic stimulation of sebum production.
Driver 2 — Abnormal follicular keratinization: Under normal conditions, the cells lining the hair follicle (keratinocytes) shed regularly and are expelled from the pore. In acne-prone skin, these cells abnormally accumulate and adhere to each other (cohesion rather than desquamation), blocking the follicle and trapping sebum. Zinc is required for normal keratinocyte differentiation — zinc-deficient skin shows abnormal follicular keratinization patterns that predispose to comedone formation. Vitamin A (retinol), which requires zinc for its binding protein synthesis, is the primary regulator of keratinocyte differentiation.
Driver 3 — Cutibacterium acnes proliferation: C. acnes (formerly Propionibacterium acnes) is a normal resident of the skin microbiome that becomes pathogenic when it proliferates in the anaerobic, sebum-rich environment of a blocked follicle. C. acnes metabolizes sebum triglycerides to fatty acids that irritate the follicle wall and activates TLR2 and TLR4 (toll-like receptors) on keratinocytes and macrophages — triggering the inflammatory cascade that transforms a comedone into a papule, pustule, or nodule. Zinc has direct antimicrobial activity against C. acnes — both topical zinc and serum zinc from dietary sources reduce C. acnes proliferation through mechanisms including disruption of bacterial membrane function and inhibition of bacterial lipase activity.
Driver 4 — Inflammatory immune response: The inflammatory response to C. acnes and blocked follicles is mediated by IL-1β, TNF-alpha, IL-6, and IL-8 — with NF-kB as the master transcriptional regulator of this inflammatory cascade. Zinc directly inhibits NF-kB activation, suppresses inflammatory cytokine production, and reduces the oxidative stress that amplifies the inflammatory response in sebaceous tissue. Zinc-deficient states are specifically associated with elevated IL-1β and TNF-alpha production, explaining why zinc deficiency worsens inflammatory acne severity independently of sebum and bacterial effects.
The Hormonal Dimension: IGF-1, Insulin, and Androgens
The hormonal drivers of acne extend beyond DHT. Insulin-like growth factor 1 (IGF-1), stimulated by high-glycemic-index foods and dairy consumption, acts on sebaceous glands through IGF-1 receptors and also stimulates adrenal androgen production — amplifying the androgenic sebum stimulation that DHT produces. Research published in the Journal of the Academy of Nutrition and Dietetics has directly linked dietary glycemic load to acne severity, with high-GI diets consistently worsening acne outcomes in intervention trials.
Insulin resistance — produced by chronically elevated dietary glycemic load — reduces sex hormone binding globulin (SHBG) production, increasing the proportion of free (bioavailable) testosterone and DHT. This creates a second pathway by which high-GI dietary patterns worsen acne through hormonal mechanisms that operate entirely independently of zinc.
Understanding these multiple simultaneous drivers explains why a comprehensive dietary approach — zinc-rich foods combined with low-glycemic eating, adequate omega-3s, and supporting micronutrients — produces more significant clinical outcomes than any single dietary intervention alone.
Why Zinc Status Matters: The Research Picture
A systematic review and meta-analysis published in BioMed Research International confirmed that serum zinc levels are significantly lower in acne patients than in healthy controls — with the magnitude of deficiency correlating with acne severity. Patients with severe acne had lower zinc levels than those with moderate acne, who had lower levels than those with mild acne — establishing a dose-response relationship that strongly implicates zinc deficiency as a causally relevant factor rather than an incidental association.
Multiple randomized controlled trials have tested oral zinc supplementation against standard acne treatments:
A landmark trial compared zinc gluconate (30mg elemental zinc daily) to minocycline (100mg daily) — a standard oral antibiotic for acne — and found that zinc produced 49% reduction in inflammatory lesion count compared to 63% for minocycline. While zinc was slightly less potent, it produced equivalent outcomes in a subset of patients while carrying none of the antibiotic-related risks (resistance, gastrointestinal disruption, photosensitivity, Clostridioides difficile risk).
Earlier trials comparing zinc to tetracycline found comparable efficacy at matching zinc doses — with zinc outperforming placebo consistently across all trial arms and producing significant reductions in both inflammatory and non-inflammatory lesion counts within 12 weeks of supplementation.
The 15 Best Zinc-Rich Foods for Acne
1. Oysters
Oysters are, without contest, the most zinc-dense food available in the human diet — providing more zinc per serving than any other food by a substantial margin, making them a uniquely powerful dietary zinc intervention for acne management.
How it works: A six-oyster serving (approximately 85g) provides 32–74mg of zinc — up to 670% of the daily recommended intake (11mg for adult men, 8mg for adult women). This extraordinary zinc concentration reflects oysters' role as filter feeders in zinc-rich marine environments, bioaccumulating zinc at concentrations far exceeding any terrestrial food source. The zinc in oysters is highly bioavailable — the heme iron co-presence in shellfish and the absence of phytate (the plant compound that binds zinc and reduces absorption) means oyster zinc is absorbed at rates of 20–40%, compared to 10–15% for plant food zinc.
Oysters also provide copper (required in 1:8 ratio with zinc to prevent copper-zinc competitive inhibition), selenium (antioxidant synergist with zinc in skin), and vitamin B12 and iron — making them a nutritionally comprehensive skin health food beyond their extraordinary zinc density.
Research on shellfish and skin health consistently identifies oysters as the most efficient dietary source for raising serum zinc in deficient individuals — with a single serving providing more zinc than multiple days of plant-based dietary intake combined.
How to use it: Two to four oysters, two to three times weekly, provides meaningful zinc supplementation through food. Raw oysters on the half shell, steamed, or grilled. Canned smoked oysters are a highly accessible and economical form with comparable zinc content. Add to pasta dishes, soups, or eat as an appetizer. For those who genuinely cannot tolerate oysters, the zinc hierarchy continues with the foods below — but no other food comes close to oyster zinc density.
2. Beef and Lamb (Grass-Fed)
Red meat — particularly beef and lamb — provides the most zinc of any commonly consumed everyday food, alongside the complete amino acid spectrum and heme iron that maximize zinc absorption through competitive facilitation rather than competition.
How it works: A 3-ounce serving of beef chuck provides approximately 7mg of zinc — 64% of the daily recommended intake for men, 87% for women — in the highly bioavailable heme-associated form. Grass-fed beef provides higher omega-3 fatty acid content than grain-fed (the ratio of omega-3 to omega-6 is approximately 1:2 in grass-fed vs. 1:20 in conventional grain-fed beef), directly relevant to acne because omega-6 dominance drives the arachidonic acid cascade that amplifies sebaceous gland inflammation.
Lamb provides comparable zinc to beef (approximately 6mg per 3oz serving) with a naturally more favorable omega-3 profile even in conventional production, making it a nutritionally preferable red meat choice for acne management when grass-fed beef is unavailable or unaffordable.
Zinc from red meat does not require consideration of phytate inhibition, fiber competition, or the conversion limitations that apply to plant-based zinc sources — the bioavailability is direct and predictable. Including red meat two to three times weekly provides a reliable zinc foundation that is difficult to replicate through plant foods alone without strategic dietary planning.
How to use it: Lean cuts of grass-fed beef (sirloin, eye of round, chuck) or lamb two to three times weekly as a dinner protein. Combine with zinc-supportive micronutrients: garlic (selenium), leafy greens (vitamin A precursors), and olive oil (anti-inflammatory) for a meal specifically assembled for skin health. Avoid processed red meat (sausages, hot dogs, bacon) — the sodium, nitrates, and preservatives in processed forms produce systemic inflammation that counteracts zinc's anti-inflammatory skin benefits.
3. Pumpkin Seeds (Pepitas)
Pumpkin seeds are the most zinc-dense plant food — providing the highest zinc concentration of any nut or seed alongside selenium, magnesium, and the anti-inflammatory gamma-linolenic acid that makes them a comprehensive skin health seed.
How it works: One ounce of pumpkin seeds provides 2.2mg of zinc — 20% of the daily recommended intake — alongside 168mcg of selenium (the antioxidant mineral that works in direct synergy with zinc to quench the reactive oxygen species that drive skin inflammation) and significant magnesium and iron. While pumpkin seed zinc is less bioavailable than oyster or beef zinc (phytate content reduces plant zinc absorption), soaking or sprouting pumpkin seeds reduces phytate by 30–50%, meaningfully improving zinc bioavailability from this source.
The gamma-linolenic acid (GLA) in pumpkin seeds is converted to DGLA (dihomo-gamma-linolenic acid), which is metabolized to prostaglandin E1 — an anti-inflammatory prostaglandin that directly counteracts the pro-inflammatory prostaglandin E2 (from arachidonic acid) that drives sebaceous gland inflammation and sebum overproduction. This makes pumpkin seeds a dual zinc + anti-inflammatory intervention for acne.
How to use it: Two tablespoons of raw or lightly toasted pumpkin seeds daily — on salads, in trail mix, as a standalone snack, or blended into smoothies (pepita powder). Soak overnight and dry-roast for maximum zinc bioavailability. Pumpkin seed butter (2 tablespoons) provides comparable zinc in a more versatile form. Combine with a vitamin C source (lemon juice dressing, bell peppers) — vitamin C enhances non-heme zinc absorption by reducing phytate-zinc binding.
4. Chicken and Turkey (Dark Meat)
Poultry provides highly bioavailable zinc in concentrations that make it one of the most practical everyday zinc sources for acne management — with dark meat (thigh, drumstick) providing nearly double the zinc of white meat (breast) from the same animal.
How it works: A 3-ounce serving of chicken thigh provides approximately 2.7mg of zinc, compared to 1.0mg from chicken breast — the myoglobin-rich dark meat tissue accumulates zinc at higher concentrations because zinc is involved in the oxygen-handling enzymes of aerobic (dark meat) muscle tissue. Turkey dark meat provides comparable zinc (2.5mg per 3oz) with the same bioavailability advantage of heme-proximate animal protein zinc.
Both chicken and turkey provide the tryptophan → serotonin pathway that supports skin through stress hormone modulation (cortisol is a potent sebaceous gland stimulant — the stress-acne connection is real and hormonally mediated) and the B vitamins (particularly B6) required for zinc's enzymatic cofactor functions in skin. B6 is specifically required for the enzyme delta-6-desaturase, which converts dietary linoleic acid to GLA — directly supporting the anti-inflammatory fatty acid pathway described in pumpkin seeds.
How to use it: Include chicken thighs or turkey drumsticks two to four times weekly. Bone-in, skin-on preparations retain more zinc than heavily processed boneless preparations. Roast with garlic (selenium), turmeric (NF-kB inhibition), and olive oil (anti-inflammatory) for a skin-supportive meal. For meal prep, chicken thigh is significantly more zinc-dense than chicken breast per calorie — prioritize dark meat when zinc optimization is the goal.
5. Hemp Seeds
Hemp seeds provide the most complete and bioavailable plant-based zinc source alongside the ideal omega-6:omega-3 fatty acid ratio that makes them uniquely suited to the inflammatory dimension of acne management among plant foods.
How it works: Three tablespoons of hemp seeds provide 3mg of zinc — 27% of the daily recommended intake — in a protein matrix that is more bioavailable than most plant zinc sources due to the relatively low phytate content of hemp compared to legumes and whole grains. Hemp seeds are unusual among plant zinc sources for this lower phytate interference.
The omega-6:omega-3 ratio of hemp seeds (approximately 3:1) is considered optimal for anti-inflammatory fatty acid metabolism — supporting the conversion of dietary omega-3 ALA to EPA and DHA without the excessive omega-6 competition that characterizes most plant oils and seeds. EPA and DHA directly reduce the leukotriene B4 and prostaglandin E2 production that drives sebaceous gland inflammation and the inflammatory phase of acne lesion development.
Hemp seeds also provide gamma-linolenic acid (GLA) — the anti-inflammatory omega-6 that, unlike linoleic acid, follows the anti-inflammatory prostaglandin E1 pathway. GLA is found in few foods (hemp seeds, evening primrose oil, borage oil) and is specifically relevant to acne because research has shown that acne patients have impaired delta-6-desaturase activity — the enzyme that converts linoleic acid to GLA — meaning they derive less anti-inflammatory GLA from their dietary omega-6 intake than clear-skinned individuals, and dietary GLA directly compensates for this enzymatic deficit.
How to use it: Three tablespoons of hemp seeds daily — sprinkled on oatmeal, salads, smoothies, or yogurt. Hemp seeds require no preparation and are fully digestible whole, unlike flaxseed. Hemp seed protein powder (for those seeking higher concentrated zinc from hemp) provides comparable zinc in a more concentrated form. Store in the refrigerator to prevent fatty acid oxidation.
6. Legumes (Chickpeas, Lentils, Black Beans)
Legumes are the most zinc-dense plant food category for vegan and vegetarian acne management — providing meaningful zinc alongside the specific fiber compounds that modulate gut microbiome composition and the gut-skin axis that connects digestive health to skin inflammatory status.
How it works: One cup of cooked chickpeas provides 2.5mg of zinc; lentils provide 2.5mg; black beans 1.9mg — each representing 20–23% of daily recommended intake. While phytate content in legumes significantly reduces zinc bioavailability (typically 10–15% absorption compared to 20–40% for animal sources), systematic phytate reduction through soaking (soak dried legumes for 12–24 hours, discard soaking water), sprouting, and fermentation dramatically improves zinc bioavailability — sprouting legumes for 48–72 hours can reduce phytate by 50–75% and increase zinc bioavailability to approach animal source efficiency.
The gut-skin axis — the bidirectional communication between gut microbiome and skin immune function — is directly relevant to acne pathogenesis. Research published in the Journal of Clinical Medicine has established associations between gut dysbiosis and acne severity, with the specific mechanism involving increased intestinal permeability → systemic LPS (bacterial endotoxin) exposure → activation of the same TLR4 receptor pathways that C. acnes activates in skin. Legume fiber (particularly resistant starch) feeds the butyrate-producing gut bacteria that maintain intestinal tight junction integrity, reducing the systemic inflammatory endotoxin load that amplifies skin inflammation.
How to use it: One to two cups of cooked legumes daily. Soak dried legumes for 12 hours before cooking — this single step meaningfully improves zinc bioavailability. Hummus (blended chickpeas + tahini + lemon) combines chickpea zinc with tahini zinc and lemon vitamin C for enhanced absorption. Combine with vitamin C sources at every legume-containing meal (tomatoes, bell peppers, lemon juice) — vitamin C is the most effective single dietary strategy for improving non-heme zinc absorption.
7. Eggs
Eggs provide highly bioavailable zinc alongside the full spectrum of skin-critical micronutrients — vitamin A (as retinol, the most bioavailable form, directly regulating keratinocyte differentiation), selenium, B vitamins including biotin, and sulfur amino acids that are direct precursors for glutathione — the skin's primary antioxidant.
How it works: Two whole eggs provide approximately 1.3mg of zinc — 12% of daily recommended intake — in a highly bioavailable form free from phytate interference. The zinc in eggs is primarily concentrated in the yolk (the white contains negligible zinc) alongside the cholesterol that serves as the direct precursor for testosterone and adrenal steroid synthesis — relevant context, though dietary cholesterol has minimal impact on sex hormone production in most people.
The retinol content of egg yolks (approximately 80mcg per yolk) is directly relevant to acne: retinol is converted in skin cells to retinoic acid (the biologically active form of vitamin A), which regulates keratinocyte differentiation in the follicle lining and is the same mechanism by which prescription retinoids (tretinoin, adapalene) work topically. Zinc is required for the synthesis of retinol-binding protein (RBP) — the transport protein that carries retinol from the liver to skin cells. In zinc deficiency, retinol-binding protein synthesis is impaired and vitamin A becomes functionally unavailable to skin tissue even when dietary vitamin A intake is adequate — creating a secondary vitamin A deficiency through zinc-dependent transport failure.
Selenium in eggs (15mcg per egg) works synergistically with zinc — both are required for glutathione peroxidase, the enzyme that neutralizes the hydrogen peroxide and lipid peroxides that trigger inflammatory signaling in sebaceous tissue.
How to use it: Two whole eggs daily — always including the yolk for retinol, zinc, selenium, and biotin. Prepare in olive oil or butter (fat enhances retinol absorption) with garlic and spinach for a skin-supportive breakfast stacking zinc, retinol, selenium, vitamin C (spinach), and anti-inflammatory monounsaturated fat. Avoid discarding yolks — the egg white has no meaningful zinc, retinol, or selenium.
8. Pumpkin (and Winter Squashes)
Pumpkin flesh and seeds together provide one of the most skin-comprehensive foods available — combining the zinc of the seeds with the beta-carotene (provitamin A) of the flesh in a single food category that addresses both the zinc and vitamin A dimensions of acne management simultaneously.
How it works: Pumpkin flesh provides extraordinarily high beta-carotene — approximately 4,120mcg per cup cooked, providing over 400% of the vitamin A daily requirement when converted to retinol equivalents. Beta-carotene is the plant precursor to retinol, converted in the intestinal wall and liver by the enzyme beta-carotene-15,15'-monooxygenase (BCMO1). Critically, this conversion is impaired in a significant proportion of the population by common polymorphisms in the BCMO1 gene — individuals with these variants convert beta-carotene to retinol at only 10–20% efficiency compared to standard conversion. For these individuals (estimated at 30–45% of the population), plant beta-carotene is a poor retinol substitute and preformed retinol from animal sources (egg yolks, liver, dairy) is essential.
The combination of beta-carotene (for those who convert efficiently) + pumpkin seed zinc creates a within-category food synergy for the two most skin-specific nutrients in acne management. Roasting pumpkin seeds with pumpkin flesh in olive oil (fat dramatically increases beta-carotene absorption — carotenoids are fat-soluble) creates a preparation that maximizes the bioavailability of both.
How to use it: Roasted pumpkin or butternut squash (drizzled with olive oil for beta-carotene absorption) alongside a tablespoon of pumpkin seeds — 2–3 times weekly as a side dish or salad base. Pumpkin soup blended with olive oil or coconut milk provides highly bioavailable beta-carotene in a warming, satiating form. Pumpkin puree (unsweetened, not pumpkin pie filling) can be added to overnight oats, smoothies, or sauces for daily beta-carotene delivery.
9. Cashews
Cashews provide the highest zinc of any common nut (excluding the seeds), alongside copper in the biologically required ratio with zinc, making them the most zinc-complete nut for sustained daily supplementation of zinc through food.
How it works: One ounce of cashews provides 1.6mg of zinc — 15% of daily recommended intake — alongside 0.6mg of copper. The zinc-copper ratio in cashews (approximately 2.7:1) is close to the physiologically recommended 8:1–10:1 dietary ratio — relevant because zinc and copper compete for intestinal absorption through the same transporter (metallothionein). High zinc intake without proportional copper increases risk of secondary copper deficiency, producing the paradox of zinc supplementation worsening some inflammatory conditions through copper-mediated ceruloplasmin reduction. Whole food zinc sources like cashews naturally deliver both minerals in supportive ratios.
Cashews additionally provide magnesium (83mg per oz), which supports the HPA axis regulation relevant to cortisol-driven acne — chronic stress raises cortisol, which stimulates both sebaceous gland activity and androgen production, connecting psychological stress to acne severity through a fully biochemical pathway that magnesium dampens.
How to use it: One ounce of raw or lightly roasted cashews as a daily snack. Cashew butter (two tablespoons) on whole grain toast provides zinc alongside low-glycemic carbohydrate — avoiding the blood glucose spikes that would elevate IGF-1 and worsen acne through the hormonal pathway. Combine cashews with pumpkin seeds (for selenium complement) and dried tart cherries (for anti-inflammatory anthocyanins) as a daily skin health trail mix.
10. Sardines and Canned Fish (Salmon, Tuna)
Sardines represent the most nutritionally comprehensive skin health fish — providing zinc, omega-3 EPA and DHA, vitamin D, selenium, and calcium (from edible bones) in a combination that simultaneously addresses the inflammatory, hormonal, and oxidative dimensions of acne in one whole food.
How it works: A 3-ounce serving of sardines provides 1.3mg of zinc alongside 1,400mg of EPA+DHA combined — the long-chain omega-3 fatty acids that directly inhibit the inflammatory leukotriene B4 and prostaglandin E2 that drive sebaceous gland inflammation and acne lesion severity. Research published in Lipids in Health and Disease has established that EPA specifically reduces the production of the inflammatory eicosanoids that amplify acne pathogenesis by competitively displacing arachidonic acid from COX and LOX enzyme active sites.
Vitamin D from sardines (approximately 270 IU per 3oz serving) is directly relevant to acne because vitamin D receptors are expressed in sebaceous glands and keratinocytes, where vitamin D signaling regulates both keratinocyte differentiation (abnormal differentiation is acne driver 2) and the antimicrobial peptide production (cathelicidins) that constitute the skin's innate immune defense against C. acnes proliferation. Vitamin D deficiency is independently associated with acne severity in multiple cross-sectional studies.
Selenium from sardines (45mcg per 3oz) completes the zinc-selenium antioxidant partnership — both are required for the glutathione peroxidase and thioredoxin reductase enzymes that quench the skin inflammatory reactive oxygen species driving acne progression.
How to use it: Two to three servings of sardines or salmon weekly as an evening protein. Canned sardines in water or olive oil are nutritionally equivalent to fresh and significantly more economical — drain, rinse, and serve on whole grain crackers or in salads. Combine with leafy greens (vitamin A precursors), lemon (vitamin C, zinc absorption), and olive oil (anti-inflammatory) for a comprehensive skin health meal.
11. Whole Grains (Quinoa, Oats, Brown Rice)
Whole grains provide meaningful zinc alongside the low glycemic response that prevents the IGF-1 and insulin spikes that drive hormonal acne — making them the foundation carbohydrate choice for a skin-clearing dietary pattern.
How it works: One cup of cooked quinoa provides 2mg of zinc — 18% of daily recommended intake — with the additional distinction that quinoa is a complete protein (all essential amino acids), providing the full amino acid spectrum needed for collagen synthesis, barrier repair, and immune function in skin tissue. Oats provide 1.5mg of zinc per cup cooked alongside beta-glucan fiber that feeds Lactobacillus and Bifidobacterium — the gut bacteria that reduce systemic endotoxin levels and support the gut-skin axis. Brown rice provides 1.2mg of zinc per cup with the lowest glycemic response of common grains.
Critically, whole grain zinc is bound to phytate — but the phytate content of oats is significantly lower than legumes, and soaking oats overnight (to make overnight oats) activates phytase enzymes that break down phytate and improve zinc bioavailability by 20–40%. Fermenting grain products (sourdough bread uses Lactobacillus fermentation that degrades phytate) similarly improves mineral bioavailability.
The low-glycemic property of whole grains is directly relevant to acne through the IGF-1 pathway: high-glycemic foods (white bread, white rice, sugary breakfast cereals) spike insulin and IGF-1, both of which activate sebaceous gland androgen receptors and stimulate sebum overproduction through pathways entirely independent of — and additive to — zinc's DHT-5-alpha-reductase inhibition. Replacing refined grains with whole grains addresses the hormonal acne driver while simultaneously providing meaningful dietary zinc.
How to use it: Quinoa, oats, or brown rice as the primary carbohydrate foundation daily. Overnight oats (soaked 8+ hours in water or plant milk before refrigerating) for breakfast — soaking activates phytase and significantly improves zinc and mineral bioavailability while providing beta-glucan for gut microbiome support. Sourdough bread (genuine long-ferment sourdough, not commercial sourdough-flavored bread) as the bread choice — phytate-reduced by fermentation, lower glycemic response than standard bread.
12. Dark Leafy Greens (Spinach, Kale, Swiss Chard)
Dark leafy greens are the most comprehensive micronutrient package for skin health among vegetables — providing beta-carotene, vitamin C (zinc absorption enhancer), folate (for the methylation reactions that regulate skin gene expression), magnesium, and modest zinc in a fiber-rich matrix that supports the gut-skin axis.
How it works: One cup of cooked spinach provides 1.4mg of zinc alongside 840mcg of beta-carotene, 245mg of folate, and 157mg of magnesium. Kale provides similar zinc with higher vitamin C (80mg per cup cooked, raw kale even higher) — the vitamin C in kale is the most relevant component for zinc absorption enhancement, as ascorbic acid reduces zinc-phytate binding by chelating the iron that catalyzes phytate-zinc complexing.
Folate from dark leafy greens supports the methylation cycle that produces SAMe — the universal methyl donor required for the synthesis of phosphatidylcholine (cell membrane integrity), creatine, and the methylation of histamine (histamine excess is associated with skin flushing and inflammatory amplification in acne-prone skin). Magnesium from leafy greens supports HPA axis regulation and cortisol dampening relevant to stress-driven acne.
The nitrates in dark leafy greens (particularly spinach, arugula, Swiss chard) are converted to nitric oxide, which improves skin circulation and nutrient delivery to the dermis — indirectly supporting the delivery of zinc, vitamin A, and omega-3s to the sebaceous gland and follicle tissue where they exert their anti-acne effects.
How to use it: Two to three cups of dark leafy greens daily — rotate between spinach, kale, arugula, Swiss chard, and dandelion greens for diverse phytochemical coverage. Raw kale salads (massaged with lemon and olive oil) provide maximum vitamin C alongside moderate zinc and beta-carotene. Cooked spinach with garlic and olive oil is a highly bioavailable zinc + beta-carotene preparation (fat increases carotenoid absorption). Add raw spinach to smoothies (nutritionally invisible in flavor behind fruit) for daily zinc and folate delivery.
13. Tofu and Tempeh
Tofu and tempeh provide the most practically significant zinc amounts among plant proteins for vegan acne management — with tempeh's fermented form offering dramatically improved zinc bioavailability compared to non-fermented soy and most other plant protein sources.
How it works: Half a cup of firm tofu provides 1mg of zinc; half a cup of tempeh provides 1.7mg — and tempeh's fermented nature is crucial. During tempeh fermentation by Rhizopus oligosporus, the mold produces phytase enzymes that break down the phytate in soybeans, reducing phytate-zinc binding and improving zinc bioavailability significantly compared to tofu (which is not fermented) or plain cooked soybeans. Fermentation also increases the bioavailability of all minerals in the soybean matrix.
Tempeh additionally provides isoflavones (genistein and daidzein) that have mild anti-androgenic activity — potentially relevant to the androgen-mediated sebum production driver of acne, though the clinical significance of dietary isoflavone levels for acne management is less established than zinc's direct 5-alpha-reductase inhibition. Soy isoflavone effects on androgen-related acne are particularly discussed in the context of hormonal acne in women, where modest estrogen-modulating effects may reduce androgen dominance.
The complete protein in tempeh (all essential amino acids) provides the full amino acid spectrum for skin collagen synthesis, barrier protein production, and immune function — critical for the skin repair that follows acne lesion resolution.
How to use it: Tempeh two to three times weekly, marinated and pan-fried or baked. Marinating in lemon juice (vitamin C), tamari, and garlic before cooking improves zinc bioavailability (vitamin C), adds antimicrobial allicin (garlic, relevant to gut microbiome and skin immune function), and provides flavor that makes tempeh genuinely enjoyable rather than simply functional. Tofu scrambled with turmeric, spinach, and garlic provides a skin-supportive high-protein breakfast with zinc, beta-carotene, folate, and NF-kB inhibition.
14. Nuts (Brazil Nuts, Almonds, Walnuts)
Brazil nuts deserve specific mention in any acne-focused nutrition guide not primarily for their zinc content but for their extraordinary selenium density — and selenium's specific, critical role in the zinc-selenium antioxidant system that protects sebaceous tissue from the oxidative stress that amplifies every acne driver.
How it works: Two Brazil nuts provide 200mcg of selenium — well above the daily recommended intake of 55mcg, and approaching but not exceeding the upper tolerable intake of 400mcg. Selenium is required as a cofactor for glutathione peroxidase (alongside zinc) and for thioredoxin reductase — both of which neutralize the hydrogen peroxide and lipid peroxides produced during inflammatory immune responses in skin. Selenium deficiency specifically worsens the oxidative phase of acne inflammation, converting mild inflammatory lesions to more severe nodular and cystic forms through unchecked reactive oxygen species accumulation.
Almonds provide 0.9mg of zinc per ounce alongside vitamin E — the fat-soluble antioxidant that protects sebum from oxidative rancidification. Rancid (oxidized) sebum is more comedogenic and more irritating to follicle walls than fresh sebum — vitamin E in sebum is a direct protective factor against comedone-promoting oxidative sebum degradation. Low vitamin E status is associated with acne severity in research, and almonds are among the highest dietary sources of alpha-tocopherol.
Walnuts provide the ALA omega-3 fatty acid precursor alongside ellagitannins that are converted to urolithins — anti-inflammatory compounds with emerging evidence for skin barrier support. Walnuts' omega-3 content contributes to the EPA/DHA pool (through limited conversion) that reduces inflammatory prostaglandin production in sebaceous tissue.
How to use it: One Brazil nut daily for selenium (two if dietary selenium is otherwise limited — do not exceed two regularly due to toxicity risk at high selenium doses). One ounce of almonds daily for vitamin E and zinc. A small handful of walnuts daily for ALA omega-3. This three-nut daily combination covers selenium, vitamin E, zinc, and ALA comprehensively. Store all nuts in the refrigerator to prevent fatty acid oxidation.
15. Liver and Organ Meats
Beef liver is the most nutrient-dense food available for skin health — providing the highest concentrations of retinol (preformed vitamin A), zinc, copper, selenium, and B vitamins of any food, in the most bioavailable forms available from any dietary source.
How it works: Three ounces of beef liver provides 4.5mg of zinc, 6,582mcg of retinol (preformed vitamin A — not beta-carotene, but the immediately bioavailable form that directly serves skin function without requiring the BCMO1 conversion that affects 30–45% of the population), 28mcg of selenium, significant copper (in appropriate ratio with zinc), and extraordinarily high B2, B3, B5, B6, B9 (folate), and B12. This micronutrient density makes liver arguably the single most comprehensive food for addressing the full spectrum of nutritional factors implicated in acne.
The preformed retinol in liver is the same molecule used in prescription vitamin A derivatives (isotretinoin is 13-cis-retinoic acid; tretinoin is all-trans-retinoic acid) — and while dietary retinol concentrations from occasional liver consumption are far below pharmaceutical doses, the regular dietary supply of preformed retinol ensures that the retinoid-dependent processes of keratinocyte differentiation and sebum regulation have adequate vitamin A substrate even in individuals with impaired beta-carotene conversion.
Liver consumption is associated with the highest dietary vitamin A and zinc density of any food, and traditional cultures with high organ meat consumption universally demonstrate the excellent skin health that researchers have attributed in part to the extraordinary micronutrient density of these foods.
Caution: Liver is extremely high in retinol — pregnant women should limit liver to once weekly due to teratogenic risk of vitamin A excess. For non-pregnant adults, once or twice weekly is nutritionally optimal without toxicity risk.
How to use it: Two to three ounces of beef liver once or twice weekly — pan-fried with onions, garlic, and lemon juice in olive oil. The classic liver-and-onions preparation is nutritionally justified: onions provide quercetin and sulfur compounds, garlic provides selenium, lemon provides vitamin C, and olive oil provides the fat that optimizes fat-soluble vitamin (retinol, vitamin E) absorption. For those who strongly dislike liver flavor: liver pâté, liverwurst, or desiccated liver capsules (whole-food liver supplements) provide equivalent nutrition in more palatable forms.
Beyond Zinc: The Complete Skin-Clearing Nutritional Strategy
The Anti-Acne Dietary Pattern
The zinc-focused foods described above are most effective when embedded in a broader dietary pattern that simultaneously addresses the hormonal, inflammatory, and gut microbiome drivers of acne:
Low-glycemic carbohydrate selection: Replace refined carbohydrates (white bread, white rice, sugary drinks, breakfast cereals) with whole grain alternatives (quinoa, oats, brown rice, sourdough bread). The IGF-1 and insulin reduction from low-glycemic eating is additive to zinc's 5-alpha-reductase inhibition — both reduce androgen-driven sebum production through different mechanisms.
Dairy considerations: The relationship between dairy and acne is real but nuanced. Whey protein (from milk and dairy) specifically stimulates IGF-1 production — skim milk more than whole milk, because the fat in whole dairy partially blunts the glycemic response. Research published in the Journal of the American Academy of Dermatology has found associations between skim milk consumption and acne that are not replicated for whole-milk fermented dairy (yogurt, kefir). The fermentation process reduces whey content and IGF-1-stimulating activity while adding skin-supportive probiotics. Consider reducing skim milk and whey protein supplements while retaining fermented dairy.
Omega-3 fatty acid optimization: Aim for a dietary omega-6:omega-3 ratio below 5:1 (most Western diets are 15–20:1). This requires actively increasing omega-3 sources (fatty fish, walnuts, chia seeds, flaxseed, hemp seeds) while reducing omega-6 sources (vegetable oils: soybean, corn, sunflower, safflower — replace with olive oil and avocado oil).
Antioxidant-rich colorful vegetables: Lycopene (tomatoes, watermelon), astaxanthin (salmon, shrimp), lutein (kale, spinach), and zeaxanthin (orange bell peppers, eggs) all protect skin from UV-induced oxidative stress that worsens inflammatory acne.
Zinc Absorption Maximizers
Regardless of which zinc-rich foods you prioritize, several dietary strategies significantly improve the zinc you absorb from what you eat:
Vitamin C with every zinc-rich meal: 50–100mg of vitamin C (half a lemon, a small orange, half a bell pepper) reduces phytate-zinc chelation and improves non-heme zinc absorption by 30–50%. The effect is most significant for plant-based zinc sources.
Avoid calcium with zinc: Calcium and zinc compete for the same intestinal transporter. Consuming dairy or calcium supplements at the same meal as zinc-rich foods reduces zinc absorption by up to 50% at high calcium doses. Space calcium-rich foods (dairy) away from zinc-focused meals.
Phytate reduction for plant zinc sources: Soak legumes and seeds overnight. Sprout lentils (48–72 hours). Use sourdough bread. Cook oats (particularly overnight oats with extended soaking) — each strategy reduces phytate-zinc binding and improves non-heme zinc bioavailability.
Avoid coffee and tea within 60 minutes of zinc-rich meals: Tannins in tea and coffee reduce zinc absorption. The effect is less dramatic than phytate but meaningful for those relying on plant zinc sources.
Frequently Asked Questions
How much zinc do I need daily for acne improvement?
The recommended dietary allowance (RDA) for zinc is 11mg daily for adult men and 8mg for adult women. Clinical trials showing acne benefit used zinc doses of 30–90mg elemental zinc daily — significantly above RDA levels that would require supplementation to achieve. However, the dietary zinc goal for acne is not necessarily to reach clinical trial supplementation doses but to: (1) correct deficiency (serum zinc below 70mcg/dL) through consistent dietary zinc prioritization and (2) optimize zinc status to the upper end of normal range (80–110mcg/dL) through diet and modest supplementation if needed. A zinc-rich diet consistently providing 15–20mg daily from whole foods — combined with zinc supplementation of 15–30mg if serum levels are below optimal — is a practical and safe target. Do not supplement zinc above 40mg daily without medical supervision — excess zinc causes nausea, impairs copper absorption, and can paradoxically worsen acne through copper-deficiency inflammatory effects.
How long before dietary zinc changes improve acne?
Clinical trials show meaningful acne lesion count reductions at 8–12 weeks of consistent zinc supplementation. Dietary changes (as opposed to supplementation) require longer timelines because food-derived zinc, while more sustainable long-term, raises serum zinc levels more gradually than supplements. Realistic expectations: modest improvements in inflammatory lesion severity at 4–6 weeks of consistent zinc-rich dietary pattern; meaningful reduction in lesion count at 8–12 weeks; optimal outcomes at 16+ weeks when combined with the full dietary pattern (low-glycemic, adequate omega-3, reduced dairy). Acne is a slow-cycling condition — follicle biology operates on 6–8 week microcomedone development cycles, and dietary interventions require at least two full follicle cycles to show their full effect.
Can zinc alone clear acne, or do I need other dietary changes?
Zinc alone addresses the most specific and direct nutritional driver of acne. However, since acne has four simultaneous drivers (sebum, keratinization, C. acnes, inflammation) and multiple hormonal inputs (androgens, IGF-1, insulin, cortisol), the most significant dietary outcomes occur when zinc is part of a comprehensive dietary pattern addressing all drivers simultaneously: low-glycemic carbohydrates (IGF-1/insulin → androgens), omega-3 optimization (sebaceous inflammation → inflammatory lesion severity), adequate vitamin A (keratinocyte differentiation → comedone prevention), selenium and vitamin E (oxidative skin inflammation), gut microbiome support through fiber and fermented foods (gut-skin axis → inflammatory load), and stress management through adequate B vitamins and magnesium (cortisol → sebaceous gland stimulation). Zinc is the foundation, but the full pattern is the structure.
Should I take a zinc supplement in addition to dietary changes?
Testing serum zinc before supplementing is ideal — your healthcare provider can order serum zinc or plasma zinc as part of a nutritional panel. If serum zinc is below 70mcg/dL (deficient) or between 70–80mcg/dL (suboptimal), supplementation is appropriate alongside dietary optimization. Zinc gluconate and zinc picolinate have the best bioavailability among supplement forms. Zinc methionine (OptiZinc) has superior absorption and lower nausea incidence. Zinc oxide (common in generic supplements) has poor bioavailability. The standard supplementation dose for acne in clinical trials is 30mg elemental zinc daily. Take zinc supplements with food to reduce nausea — the most common side effect of zinc supplementation. Always supplement copper (2mg daily) when taking zinc supplements above 25mg to prevent copper deficiency through competitive inhibition.
Does diet alone work as well as antibiotics or isotretinoin for acne?
For mild to moderate acne, a comprehensive zinc-focused dietary strategy combined with the full anti-acne dietary pattern (low-glycemic, omega-3 optimized, adequate vitamin A and selenium) can produce clinically meaningful improvements that reduce or eliminate the need for antibiotics in some patients. For severe or cystic acne, isotretinoin (Accutane) remains the most effective single intervention and dietary changes should be implemented as a complement to, not replacement for, dermatological treatment. Oral antibiotics for acne produce antibiotic resistance in C. acnes and gut microbiome disruption — the case for prioritizing dietary zinc management as a first-line approach for mild-moderate acne before antibiotic prescription is evidence-based and increasingly supported by dermatological literature. Discuss integrating dietary strategies with your dermatologist.
Are there specific foods that make acne worse I should avoid?
The most evidence-supported dietary acne triggers are: (1) high-glycemic-index foods (white bread, white rice, sugary beverages, sweets) — directly spike IGF-1 and insulin, promoting androgen-driven sebum overproduction; (2) skim milk and whey protein supplements — whey stimulates IGF-1 production more potently than most foods; (3) processed and fast foods — combine high glycemic load, omega-6-rich industrial vegetable oils, and sodium in a pattern that drives every acne inflammatory driver simultaneously; (4) alcohol — impairs zinc absorption, depletes B vitamins required for skin cell turnover, and disrupts gut microbiome composition that regulates the gut-skin axis. Chocolate and iodine-rich foods have weaker and more inconsistent evidence as acne triggers and are lower priority elimination targets.
Is the zinc-acne connection relevant for hormonal acne specifically?
Yes — zinc's 5-alpha-reductase inhibition is directly relevant to hormonal acne because hormonal acne is driven by androgen excess (either absolute androgen elevation or androgen receptor hypersensitivity in sebaceous glands). By inhibiting the enzyme that converts testosterone to the more potent DHT within the sebaceous gland, zinc directly addresses the primary hormonal driver of hormonal acne. Women with PCOS-related acne, perimenstrual acne, and post-oral-contraceptive acne all have elevated androgen signaling as a core pathological mechanism — making zinc supplementation particularly relevant in these contexts. Zinc additionally supports the SPB (sex hormone binding protein) production that reduces free androgen bioavailability, and may modulate the HPA axis component of stress-driven androgen excess through magnesium-synergistic cortisol regulation.
References and Further Reading
Bowe WP & Logan AC — Gut Pathogens (2011) — Acne vulgaris, probiotics and the gut-brain-skin axis Foundational review establishing the gut-skin axis mechanism in acne pathogenesis — intestinal dysbiosis increases systemic inflammatory endotoxin (LPS) exposure through impaired gut barrier function, activating the same TLR4 inflammatory pathways that C. acnes triggers in skin tissue, with dietary fiber and probiotic strategies identified as gut-targeted acne interventions.
Dréno B et al. — Journal of the European Academy of Dermatology and Venereology (2018) — Skin microbiome and acne vulgaris: Staphylococcus, a new actor Comprehensive review of the skin microbiome's role in acne, including Cutibacterium acnes pathogenesis mechanisms (TLR2/TLR4 activation, bacterial lipase activity, inflammatory cytokine induction) and the evidence for zinc's direct antimicrobial effects on C. acnes proliferation and inflammatory cytokine production.
Gupta M et al. — BioMed Research International (2014) — Zinc Therapy in Dermatology: A Review Systematic review of the clinical evidence for zinc in acne treatment — including meta-analysis of randomized controlled trials comparing zinc supplementation to oral antibiotics (tetracycline, minocycline), establishing zinc's acne efficacy profile, optimal dosing, and mechanisms including 5-alpha-reductase inhibition, NF-kB suppression, and direct C. acnes antimicrobial activity.
Smith RN et al. — Journal of the American Academy of Dermatology (2007) — The effect of a low glycemic load diet on acne vulgaris Randomized controlled trial demonstrating that a low glycemic load diet significantly reduced total acne lesion count, inflammatory lesion count, and androgenic hormone levels compared to a high-glycemic control diet — establishing the IGF-1/insulin/androgen pathway as a clinically validated dietary mechanism in acne pathogenesis separate from and additive to zinc's effects.
About the Author
I'm Judith, a wellness enthusiast and Applied Bio Sciences and Biotechnology graduate behind BiteBrightly. With a deep-rooted belief in the healing power of food, my nutrition journey began with a personal transformation—I improved my eyesight through targeted dietary changes. This life-changing experience sparked my mission to empower others by sharing evidence-based insights into food as medicine.
Drawing on my scientific background, personal experience, and ongoing research into nutrition and health, I focus on breaking down complex health topics into clear, practical, and actionable guidance. My approach combines scientific credibility with real-world application, making evidence-based nutrition accessible to everyone.
Follow me on Pinterest for daily health tips, recipes, and wellness inspiration.
Important Notice: The information in this article is for educational purposes only and is not intended as medical advice. I am not a medical doctor, registered dietitian, or dermatologist. Acne is a medical condition that in many cases requires professional dermatological evaluation and treatment — particularly moderate-to-severe, cystic, or scarring acne. Dietary strategies are supportive interventions and should complement, not replace, dermatological care. Zinc supplementation at therapeutic doses (above 25mg daily) should be discussed with a healthcare provider — long-term high-dose zinc supplementation can cause copper deficiency and should be accompanied by copper supplementation at 2mg per 25–30mg zinc. Pregnant women should limit liver consumption to once weekly due to high retinol content. Individual responses to dietary changes vary significantly based on genetics, hormonal status, gut microbiome composition, and acne subtype. These statements have not been evaluated by the FDA.
Connect
Join our newsletter for fresh health tips
© 2026. All rights reserved.